#cptsd info
Explore tagged Tumblr posts
Text
my brain @ me: you will get your memories... when I decide they're relevant. Maybe not even then. However,,, anytime is a good time to repeat the same traumatic flashback that you already know about. I will do that more, just in case.
#osdd#cptsd#ptsd#flashbacks#memory loss#missing memories#brain only giving me the shitty stuff#and gatekeeping useful info#did
260 notes
·
View notes
Text
A lot of my trauma healing as of now is speaking or typing traumatic things that happened to me in order to process or speak out and being like huh. That did happen. And that was not good.
I feel like a lot of people picture trauma healing as doing intense EMDR sessions, but that's not all it is. You can't start healing until you recognize what happened was trauma. Even before that, you have to learn how to trust your own perception.
Before I started trauma therapy, I didn't feel like a person with a worldview. I felt like a bundle of trauma responses trapped in a human body. Now I can weigh how people treat me against my own paradigm of reasonable treatment. If they go against what is acceptable, I can act accordingly. I also can be held accountable more easily since I have a concept of how I should act in relationships, too.
#complex trauma's a bitch#some people also have to learn how to act rather than react#and measure if your response is reasonable or a reaction#bellaposting#methinks#original post#cptsd#actually cptsd#living with cptsd#ptsd recovery#ptsd awareness#complex ptsd#childhood trauma#c ptsd#trauma survivor#therapy#emdr#emdr therapy#post traumatic stress disorder#complex post traumatic stress disorder#dissociative disorder#dissociation#dpdr#actually dpdr#mental health#about us#did system#actually did#did osdd#did info
32 notes
·
View notes
Text
Hey Y’all, we are making a new intro!
We are the Botanical Gardens System! We like using this platform to basically post whatever we please in the moment. Bodily we are 20 years of age, and we would prefer having minimal interactions with minors in any dm setting. This page is safe from NSFW posts and content, so it is safe for minors to interact with, but we would much rather private dms and conversations be with other adults.
Our spam reblog account would be @botanical-gardens-system
We have a blog where we share system related songs as well: @botanics-beats
That’s where we house all posts we reblog without additional text. Pretty much everything is system-related, but it can sometimes repost other stuff.
It is generally safe to use he/him as a collectively pronoun.
Fun facts about us:
We are working on a bachelor’s in psychology and want a master’s in nursing!
It is possible we will try to become a psychology professor whilst being a PMHNP (psychiatric mental health nurse practitioner).
Since we are so big in psychology, our entire account is more psychological-science oriented to better understand our personal experiences.
We love sushi and fish in general as it is our favorite food.
A lot of us are generally agender, asexual, and aromatic, but we do have some alters who are pansexual and/or are a separate gender. Generally we are transmasc-neutral.
We are currently in a happy relationship right now!
We are traumagenic and have a headcount of at least 10-12 now.
If there are any other adult systems that would like to interact, I would be happy too!
DNI Criteria:
There is none. DNIs are kinda useless and instead I will just block you if I don’t feel like I want to interact with you, and feel free to block me if you think I am violating any of your DNI. I never check DNIs really and I’m sure not many check mine. Just please don’t be a dick.
Please just understand I do not care about syscourse. I think it is a useless argument and it’s very frustrating to know it encompasses a good 50-70% of all content I see on here. I can’t pass a post without seeing some kind of syscourse related tag, even if it never features it in the conversation of the post.






#did osdd#osdd community#actually did#osdd system#osddid#pluralgang#actually osdd#traumagenic did#did community#plural culture#did#osdd#system#cdd#system info#dissociative system#dissociation#actually dissociative#actually traumagenic#actuallyplural#actually plural#actual did#actually cptsd#system community#plural system#did system#sysblr#osdd 1b#plural community#plural positivity
39 notes
·
View notes
Text
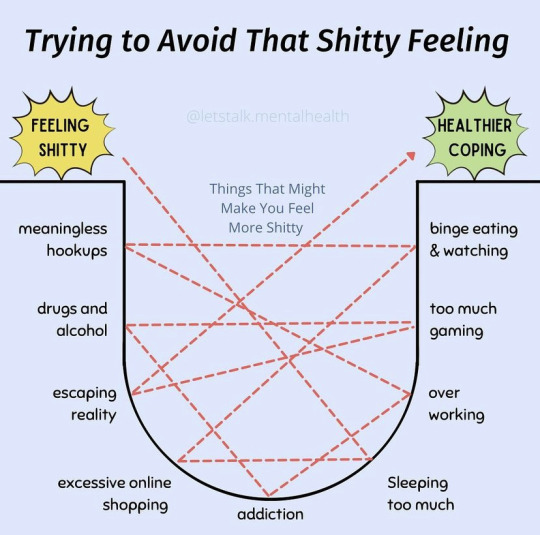

Credit
#mental health#positivity#mental illness#self care#self help#info#mental health information#recovery#pro recovery#ed recovery#actually cptsd#actuallytraumatized#actually dissociative#actually ptsd#eating disorder recovery#actuallyabused#actuallymentallyill#actuallyocd#actually autistic#actually traumagenic#trauma#childhood trauma#mentally ill#made of styrofoam#only pr0 for myself#dissociative identity disorder#obsessive compulsive disorder#inner child#ana e mia#cvtt1ng
668 notes
·
View notes
Text
So what I learned about myself by researching these topics about abuse, collected from experts and therapists who work with complex trauma patients:
Betrayal Trauma is the name of what I went through in my household
Scapegoats are often betrayed by parents and I fit the scapegoat role
Scapegoats are often “truth tellers” and fight the family narrative
Scapegoats can be betrayed by one family member OR they can be betrayed by the whole family in which the family narrative is “we are all okay and right, and you (the scapegoat) is the crazy/wrong one.”
Scapegoats often have DARVO used against them (when the abusers in the family call the scapegoat the abuser, and the real abusers/parents call themselves the victims)
Scapegoat may feel betrayed, rejected, shamed, become a people pleaser, overly forgiving, may avoid relationships and end up isolating yourself from others
Some become dependent on the abusive family as an adult, slow to get ahead in life
Toxic shame is not just feeling ashamed, but YOU ARE shame (not really true, your brain lies to you). You think You Are Shame walking around on 2 legs. (How I feel and doing my research I understand it’s the trauma brain talking but I genuinely believe the lies). “I feel humiliated when I speak in front of others” “I feel humiliated for existing and taking space”
You could have had a fight response, challenge the abusers distorted, twisted view of reality. It causes exhaustion from challenging the family false narrative growing up. You may identify with being the “fighter.”
Family Systems expert Rebecca C. Mandeville explains adult survivors of Family Scapegoating Abuse (FSA) are impacted by Betrayal Trauma. She also explains the consequences of being rejected, shamed, and blamed by the people who were supposed to love and care for you the most.
Dr. Erin Watson’s article: The Duel Layers of Betrayal Trauma for Survivors of Family Scapegoating Abuse.
#my text#cptsd life#cptsdhealing#tw cptsd#just cptsd things#cptsd vent#actually cptsd#cptsd tag#living with cptsd#cptsd problems#scapegoat#scapegoating#golden child#family systems#REALLY IMPORTANT INFO
123 notes
·
View notes
Text
Whumpee waking up absolutely drenched in sweat after having a string of nightmares based on their abuse.
Even though it's been a couple of years since everything had happened. Even though they know the dreams aren't real. But in their sleep they feel so much like recalling specific locked away memories of things they'd been through that they'd forgotten. Despite knowing they weren't actual memories of specific events and their mind has cruelly decided to make their subconscious experience new but similar events. Despite the source of the nightmares no longer being able to hurt them.
Confused, shaking and distressed in bed having woken up way earlier than they were meant to.
(MEGA Bonus points if whumpee has someone there to comfort them.)
#its me im whumpee today#whump#nightmares#text#Original#actually cptsd#please use my actual IRL experience this morning for creative pursuits#if i can't make my trauma into content or useful info for writers then WHAT'S THE POINT OF HAVING BEEN THROUGH IT?#vent#this partly counts as venting#I say it's MY turn to self comfort with hurt/comfort fiction#trauma
35 notes
·
View notes
Text
Coping Skills: Emotional Flashbacks
What are Emotional Flashbacks?
An emotional flashback is when we are triggered into living in the emotional/psychological state we experienced during our traumatic childhood experiences. We experience a regression to the emotional state of a child in trauma. This can be an experience that we are not aware of, either thinking it is about the current situation or knowing that our emotions are all over the place/disproportionate but unsure where the feelings are coming from.
Example A) You could be in a situation where you can’t easily leave (IE leaving could negatively affect a job, can not get out of a social situation or traffic). This can cause you to feel trapped. This trapped feeling is elevated beyond a normal amount and causes you to be dysregulated and negatively impacts the situation. You then might spend hours in a state of feeling trapped and the knock-on emotional effects like helplessness, fear, agitation etc. This could be because you were often or always physically or emotionally trapped in a situation of abuse as a child.
Example B) At a performance review at work you receive feedback on areas where you could improve. Instead of feeling moderately discouraged, you feel terror and shame even to the point of having trembling hands or crying. You feel a consistent level of fear hanging around. This could be because criticism or not meeting a level of “perfection” often resulted in shaming or punishment.
Emotional Flashbacks In The Brain:
When we experience chronic childhood trauma we have our neurology and biochemistry altered. So when we have external or internal reminders of our trauma those old patterns are activated. We can end up in the emotional state we were in during childhood. We are “hijacked” by our amygdala, the emotional and survival parts of our brain.
Our stress response system is activated (Fight/Flight/Freeze/Fawn) and we are thrown out of our window of tolerance (hyper/hypoarousal). The neurochemistry of our brains and the hormonal chemistry of our bodies during stressful events cause our brains to encode information differently. Experiences of trauma can leave our body unable to properly process trauma and leave us vulnerable to living in stress constantly. The change in the way our brain encodes information leads to us being able to be triggered into flashbacks.
The repeating of mental and behaviour patterns from our traumatic childhood are also in part facilitated by our Implicit Memory System.
Sings You Are In An Emotional Flashback:
When our emotions are not matching the current situation we are in or the intensity is disproportionate to what we are going through right now is a good clue that you have been triggered into an emotional flashback. Your body is flooded with the brain and body patterns of a younger you.
Common Feelings:
Childlike
Fragile
Helpless
Hopeless
Intense shame
Lost
On edge
Rage
Small
Terror
Unstable
Common Thought Patterns:
Black-and-white thinking
Can be tied to intrusive thoughts
Catastrophising
Confusion
Difficulty finding words to communicate
Distrusting people or situations you have trusted
Judgmental of other
Mind going blank
Self judgmental
Trouble interacting with other people
Common Behaviours:
Disordered eating behaviours
Binge eating
Purging
Restricted eating
Endless scrolling
Getting into fights
Getting lost in fictional stories to the detriment of your relationships and ability to to do self-care
Isolating
Utilising substances to excess:
Alcohol
Misuse of OTC medications
Misuse of prescriptions
Unregulated drugs (heroin, cocaine, etc.)
Triggers of Emotional Flashbacks:
More information and the breakdown of coping under the cut
Triggers can be internal or external and don’t even always make sense right away.
External:
Being in a place where traumatic things happened
Being drunk and/or high
Being somewhere that looks like where the trauma happened
Being with the people who were involved in trauma
Criticism
Crowds
Facial expressions or body language perceived as threatening
Facial expressions or body language perceived as disapproval or disgust
Loud voices
Media depicting events similar to your trauma
Medical with characters who remind you of the perpetrator of the abuse
Others engaged in fighting
Passive-aggressive behaviour or perceived as passive-aggressive
People who are drunk and/or high
People who look like those who traumatised you
Physical touch of any kind
Smells that remind you of trauma
Sounds that remind you of the trauma
And anything else that our brain has linked to trauma
Internal:
Daydreams that drift into visualising traumatic situations
Illness
Injuries
Intrusive thoughts
Physical pain from any source
Rumination on personal faults
Rumination of feelings of vulnerability
Thirst and hunger
and others
Coping With Emotional Flashbacks
These steps are adapted from the work of Pete Walker (LMFT)
These skills do not all need to be done every time, sometimes skipping a step might be necessary or repeating a step.
1) Say To Yourself: “I am having a flashback”
When you realise you are feeling a flashback it can feel very frightening and placing yourself in time can be very hard. You can feel helpless, by acknowledging you are in a flashback you can know you are in the now
2) Remind Yourself: “I feel afraid but I am not in danger”
You are scared, but that does not mean you are in the same place you were when you were hurt. You are in the now, and you have the power to make decisions now.
3) Own Your Right to Have Boundaries
You can explain to people that their behaviours are upsetting you. You also have the right to leave situations that are causing distress.
4) Speak to Your Inner Child
Imagine your inner child and tell yourself what you needed to hear in the past. Emotional flashbacks are pulling from past fears, your inner child deserves to be treasured with unconditional love. Tell the little you that you will be there for them now. They are not abandoned. If there are specific messages you ache to hear from others, offer those reassurances to the inner child.
5) Deconstruct Eternity Thinking
Challenge the idea that this feeling will last forever. The pain was long in the past and now you can be in charge of moving forward. Again try and hold that this is a flashback and therefore not forever.
6) Remind Yourself You Are In An Adult body
You have control now, you are bigger and can make your own choices. You have the power to act now in ways you didn’t have in the past. Like with eternity thinking you can practice reminding yourself of this regularly to increase the ability to hold this truth during flashbacks.
7) Ease Back Into Your Body
Work through the dissociative state that flashbacks put you in.
Breathe deeply: focus on the pace of our breathing and how it feels.
Gently work with your body to promote relaxation: Try progressive muscle relaxation: Tighten each muscle group starting from the feet or forehead. Breathe in and hold as you tighten and then breathe out as you release the tension
Slow down your movements: Try to reduce the stress you’re putting on your body and move out of protective mode.
Get to a safe place: If you can get to a place where you feel relatively safe and can take time to soothe your body. Warm blankets, calming music, stuffed animals, and low-sensory environments can all help.
Feel fear without acting on it: Let the energy in your body move while in a place that feels safe. Attempt to not act out to the point of harm on the strong emotions. If to remain some action is necessary try to make sure the movement is not overexercising. You want to discharge the activation without hurting yourself. and then have plenty of time to rest. The goal is to be able to feel the fear without compulsive activity or shutdown.
8) Resist Drasticizing & Catastrophizing
Use thought-stopping: When thoughts that are degrading to yourself or trying to predict that things going forward will be horrible think stop and/or say stop. Putting pressure on your body as you think it, clapping your hands, or stomping your foot can help this be effective.
Use thought substitution and correction: Over time you can learn to replace the negative thought patterns with statements you memorise to counter the automatic thoughts. Statements that promote your self-efficacy and accomplishments.
9) Allow Yourself to Grieve
If you are in a place where you are safe, bringing grief into the moment can be efficacious in reducing the power of flashbacks. Feel the emotions brought up and offer yourself compassion. It’s okay to recognize and over time validate the pain and unfairness you have faced in the past. If helpful for you can imagine consoling your inner child.
10) Cultivate Safe Relationships & Seek Support
It’s good and healthy to learn to be able to handle flashbacks on your own. However, this does not mean it’s wrong or weak to reach out to others. Co-regulation, being with another person who helps you come back to a calmer and more engaged state, can be very powerful. Having people who you can reach out to during tough times with emotional flashbacks will help you to internalise the ability to manage yourself as well as be a lifeline if your symptoms are more overwhelming than normal.
You are not a burden by asking for help and sharing what helps you cope. It is important to be reciprocal with the help if the person is a friend, partner or family member (as opposed to professionals), this does mean that needing support makes you selfish or a bad person. Healing through bonds with other people is part of being human.
11) Learn The Triggers That tend to Provoke Emotional Flashbacks
Pay attention to what situations, people and thought patterns precede emotional flashbacks. Keeping a log can often be very helpful.
It can also be efficacious to consider which of these are non-essential activities, situations, and relationships (in the case of internal feelings or thoughts that can learn to deal with). The triggers that are not necessary for your life can be avoided or minimised. It’s not cowardly or wrong to step back from things that are only causing distress and not giving you anything you need.
Things that are necessary or unavoidable can be learned to be coped with or even modified. Learning coping skills to deal with different aspects of flashbacks, anxiety, dissociation, intrusive thoughts and sensory distress is key here. Managing the symptoms will make life easier as you learn them, generally before you can get to processing the more narrative aspects of trauma. Dealing with nervous system distress and vulnerability is generally very useful to do during recovery.
You can also figure out if the situation would allow you to bring aids like fidget toys, other stimming aids, ear defenders, things to colour/write with etc. If the situation itself can be modified, like allowing you to take more breaks. You can also request to be warned if triggering subject matter, flashing lights, group projects or other triggers are going to be a part of lessons/work so you can prepare yourself.
If the situation is with a job, reaching out to HR or a disability coordinator can be helpful or if in school there are usually offices that deal with disability and accommodations. However, a diagnosed mental illness might be necessary to make these options open to you. But the above-mentioned things like stimming aids, warnings and other things might be able to be negotiated with people without a diagnosis.
If you are dealing with interpersonal relationships you can do internal work to set up boundaries. This can start with what you will do to handle specific upsets and what actions you are willing to do. If safe you can share some of your boundaries so they are aware of where you stand. And you can even figure out if they are someone you can work together with to strengthen your relationship through ongoing dialogue about boundaries and supporting one another’s health and well-being.
Dealing with people who are not going to work with you or are very hurtful to you can be very hard. One way to deal with this is to decide how much of yourself you are going to invest. If it is unavoidable that you have to be with them, like extended family or colleagues, you can back away from putting in more time and feelings. You don’t have to put in extra work or hours than you have to. You can share less of your emotional world and perspectives. Conversation can be kept to a minimum. This does not mean you need to be rude or mean, you can be polite, but you try to make your emotional wellness not tied to them.
You can also figure out what is intolerable for you, what will cause you to leave an interaction with them or even cut off contact completely. It’s good to know what behaviour violates you psychologically and/or physically. It’s important to think this through, to make sure the line is drawn at a reasonable point and that you have ways to keep yourself safe should people cross it.
12) Figure Out What You Are Flashing Back To
This step should be done with caution if you are not out of the traumatising situation (IE living with the perpetrator[s] or with other abusive parties).
What triggers flashbacks and what emotions are being experienced can give you clues as to what wounds you are carrying with you. Our community has generally experienced CSA, but it is still important to learn what emotions these experiences have left in you. Recognizing the emotion can help you work through it in conversation, writing, art, and finding the best coping skills. If you seek professional help it can lead to what treatment might work best. Knowing what feelings you have and their origin can also help you grieve and offer yourself compassion and understanding. It can make working with your inner child and/or inner world more healing.
It can help with re-parenting, if this is something you need to do, to know what deficits and abandonment you are still carrying with you.
Knowing what triggers bring up with strongest responses, and the kind of response can make metabolising these memories easier. Being able to reconnect the emotional, somatic, and narrative properties of experience can help us feel more fully human and healthy.
13) Be Patient & Kind to Yourself During Your Journey
Recovery takes different amounts and time and styles of coping for every person. The trauma was individual, your DNA and body are unique so is the help (or lack thereof) you got after the trauma. Do not be mad at yourself for having flashbacks and other trauma responses. Work to combat blaming and shaming thoughts when they come up. Let yourself move through all the facets of your story and heal as slowly or quickly as is right for you.
You can heal and will get there, and it’s okay whatever that looks like.
Citations:
Braman, L. (2022, May 5). The Difference Between Emotional Flashbacks & Flashbacks. Lindsay Braman. https://lindsaybraman.com/emotional-flashbacks/#what-are-emotional-flashbacks
Bruce Duncan Perry, & Oprah Winfrey. (2021). What happened to you? : conversations on trauma, resilience, and healing. Flatiron Books.
Davis, S. (2019, July 1). The Living Hell of Emotional Flashbacks. CPTSD Foundation. https://cptsdfoundation.org/2019/07/01/the-living-hell-of-emotional-flashbacks/
Der, V., E R S Nijenhuis, & Steele, K. (2006). The haunted self : structural dissociation and the treatment of chronic traumatization. W.W. Norton.
East Bay Therapist. (2005, October). EMOTIONAL FLASHBACKS | Healing & C-PTSD. Healing and C-PTSD. https://www.healingandcptsd.com/emotional-flashbacks
Levine, P. A. (1997). Waking the tiger – healing trauma : the innate capacity to transform overwhelming experiences. North Atlantic Books.
Levine, P. A. (2015). Trauma and memory : brain and body in a search for the living past : a practical guide for understanding and working with traumatic memory. North Atlantic Books.
Walker, P. (2021). Complex PTSD : from surviving to thriving : a guide and map for recovering from childhood trauma (first Edition). Azure Coyote.
#blog post#info#informational article#coping skills#our post#ptsd#cptsd#childhood trauma#trauma#flashbacks#emotional flashbacks#abuse recovery#trauma recovery
74 notes
·
View notes
Text
The Bear is crazy because I'll be like, "ha, damn, at least I wasn't the middle child or the youngest child in my extremely abusive household," and then the whole show is about how Mikey is DEAD by suicide and I have to get up and walk in a few circles until I remember how to breathe and then the next episode is just like, "here's 1/3rd of our run time to John Cena for some reason."
#the bear#it feels like a Fine™️ person writing about trauma as a bit#writing about cptsd the way Bear Grylls survive the wild for the TV#like this is useful info sometimes but i can tell you werent there#idk maybe the showrunner is just extremely goofy#good show#have it in just in case jail all the same
7 notes
·
View notes
Text
"In Trauma and Recovery, Herman expresses the additional concern that patients with CPTSD frequently risk being misunderstood as inherently 'dependent', 'masochistic', or 'self-defeating' [personality disorders], comparing this attitude to the historical misdiagnosis of female hysteria."
~ Wikipedia's CPTSD article






~ Judith Herman, Trauma and Recovery (2015), pp. 116-118.
Thank you to @/avoydant, who transcribed these images. The transcriptions have been added to the alt text.
#so many pds could just be subtypes of cptsd. maybe even all of them.#cptsd#pd info#judith herman#trauma and recovery#dpd#dpd info#masochistic personality disorder#self defeating personality disorder#hysteria#pds and trauma#dogpost#hpd#hpd info#passive aggressive personality disorder#negativistic personality disorder#sexism and misogyny in psychiatry#victim blaming#abuse tw#psych critical#anti psych#anti psychiatry#psychiatry critical#described#described in alt text#i was gonna just post a snippet of the section but the whole thing is important
66 notes
·
View notes
Text
Read Me Please!
Hello there fellow past, present, and sadly future foster children. This tumblr blog is where you can find out or share the horrors of living as a foster child in the child protective systems, an adoption child living in the system, working as a foster parent, caseworker, or just any terrible experience one has had in fostercare. You can also just share how you got into fostercare, thats allowed too. **Just share in the ask me!!!** Here are the rules with posting: - You are allowed to be anonymous as this is a safe place to share your stories. - You must add what year you were in foster care during the event as that will help spread awareness of how long ago or recent the story occurred. - Must be a true story. - You do not have to disclose age, gender, or what county you were in if you do not want to. - You can name drop your abusers here, no one will shame you for standing your ground and calling them out. - This is a safe space. You cannot use slurs, be racist, homophobic, nsfw, ect. Unless you are sharing what the ones in the story did. Example on what you can do: My fostermom said that I would never find love becuase I wasn't into boys like others were. - Don't be too graphic, we want our stories out there to be digestible, remember that not everyone can stomache the extreme details of what may have happened. -Be respectful and supportive of eachother. If not then this blog isn't for you. -This blog is kin friendly, endogenic friendly, traumagenic friendly, lgbtq friendly, and ect. -This blog does not accept homophobes, pedophiles, sysmeds, anti-endos, narcisists, and basuically anyone who is inconsiderate douchebags. -If your post is not posted, please know that I may just not have seen it or it did not follow the rules. -This blog is run by a former fosterchild who grew up in terrible conditions. You may see posts from this channel and if thats the case, that is me sharing my story. Reasons why this blog exists: I felt like I wanted to share my story and wanted to spread awareness on how bad the system can get, and if I had bad experiences, I'm sure many have too so I wanted to make a safe place where we can all share our stories and maybe... just maybe... the system that has hurt many can be seen by higher authorities and can be brought to their attention as an issue that must be resolved.
#my blog#rules and guidelines#rules and info#traumatic fostercare stories#foster care#fuck cps#adoption trauma#cptsd
2 notes
·
View notes
Text
This video talks about neurological dysregulation: how to cope with it, how to combat it, and how to turn a bad day into a good one.
youtube
#important#life#psychology#Childhood Fairy#tips#healing that wounded inner child#learning CPTSD info for family#Youtube
3 notes
·
View notes
Text
I think that being autistic got me fucked up
#/pos#but also like vent ish#ok to rb#system babbles#my special interest rn is things that harm me. get out of here who let that sink in#like what do you want im fascinated by the degradation of my body in response to trauma#and the internal lashing out of an already neurospicy brain under incomprehensible suffering#all living things respons in insane overdone ways in panic response and we dont have the research to fully comprehend#even physically threatening immediate situations so how fucking interesting is it to consider abstract threats and the effect that has on a#autistic brain addicted to the internet in a cptsd way with osdd with schizo symptoms and all this other stuff#on TOP of addiction in the family chronic illness EDS (and its ties to autism) and just so so so many things im so so fascinated#but i take fucking psychic damage even considering this stuff or remembering anything so autistic hyperfixation sessions get painful as hel#and i can't even leave i have to let the interest brain pick over articles and info vida until it calms down and buddy its trembling#autism#neurodivergent#special interest#psychology#inthrum bickerman#btw im still in front day 42 fucking laughing my ASS OFF TAKE THAT
4 notes
·
View notes
Text
Glass Children Info & Masterpost
Only recently being recognized as a huge trauma itself, I’ve seen nothing on Tumblr being posted about glass children. And as a glass child myself, which is a part of the reason I’ve struggled severely with mental illness, especially in my early teen years, it can be very upsetting. However, it’s still incredibly popular to view what we experience as invalid and that we should “appreciate we aren’t like them” (which is incredibly insulting to both parties and I hate hearing it). Idk if this will get any notes, but I wish someone told me what I went through is valid and a real thing and I hope maybe this will show one person the same:
Glass Child: siblings of a person with a disability. The word glass means people tend to see right through them and focus only on the person with the disability. 'Glass' is also used because the children appear strong, but in reality are not. These children have needs that are not being met.
The term was popularized and recognized in Alicia Maples’s “Recognizing Glass Children” TedTalk posted in December, 2010 in which she talks about her experience growing up with a severely Autistic brother.
It is important to acknowledge that the disabled sibling plays no role in the conditions and problems a glass child endures as they did not choose to have a disability. The conditions and problems are a product of bad parental management and being a victim of circumstances. As a child, not understanding this bigger pictures may sometimes cause a glass child to see their sibling as the problem, but it is important to stress the sibling has no part in it.
Examples of challenges glass children experience during childhood:
Severe emotional and or physical neglect from guardians
Severe pressure to be the “perfect” kid
Feeling as if you must help others before yourself
Strong anger of not having a “normal” family, but feeling shame for feeling anger.
Putting in extra effort to appear okay even when they aren’t
Taking on the tasks (both physical and or mental) that are reserved for parents
Feelings of hopelessness
Hyper-vigilance and anxiety
Feeling of being taken for granted
These experiences during childhood follow you into teenage years and adulthood.
Symptoms a glass child can show later in life:
Trauma-related mental illnesses (ex: anxiety, depression, PTSD, personality disorders, eating disorders, etc.)
Self-sabotaging or self-injurious behavior(s)
Low self esteem
Putting other’s needs before one’s own, even at their own expense
Lack of self identity or never developing their own personality
Hyper-vigilance to an inappropriate degree
Extreme sensitivity
Struggles with trust and or vocalizing feelings and needs
Difficulty in adjusting to new, unexpected situations
Avoidance of any form of conflict to the point where it has negative impacts on day to day life
Learn More:
Glass Child Syndrome And Symptoms
Glass children: The overlooked siblings of the people we treat.
What is a glass child?
How We Can All Help Glass Children
Growing Up a Glass Child
Glass Child Syndrome And Symptoms
Glass children: The lived experiences of siblings of people with a disability or chronic illness
Glass Children
At least from my experience, one of the biggest problems that follows me till this day is being extremely sensitive as to when I feel my feelings or presence is being invalidated. This is not completely my imagination however as the term “glass child” as of now has no place in the DSM-5, any dictionaries, and not even a Wikipedia page despite the years and years of studies and proof showing that the existence and damage of being a glass child is very real and a problem. I myself didn’t know about this term until a few months ago. And that was from TikTok of all places. I hope this makes at least one more person aware that we exist, we are valid, and we are not “the lucky one.” Both the disabled sibling and the glass child(s) deserve the recognition for enduring the hardships life threw at them. We both deserve it.
#mental health#positivity#mental illness#self care#self help#info#mental health information#infographic#mental health infographic#mental illness infographic#glass child#glass children#mentally ill#trauma#childhood trauma#emotional neglect#neglect#actuallyneglected#cptsd#positive vibes#self esteem#love#signal boost#urgent#information#mental health reminders#awareness#mental heath awareness#therapy#vent
137 notes
·
View notes
Text
To pick apart someone’s words to try to “catch them in a lie” or hold it against them is absurdly fucking manipulative. You’re not being perceptive, you’re just stroking your ego and being manipulative. There’s a huge difference with someone just trying to honestly explain a situation or how they feel or explaining something traumatic, you don’t get to pick them apart for their word choices, or mistakes in explanation, or their tone of voice, or their reaction being “too dramatic” or “not emotional enough” or that some of us can be quite incoherent in our speech and writing sometimes due to mental illness and to pick us apart for that is disgusting and manipulative.
#my text#REALLY IMPORTANT INFO#actually traumatized#actually cptsd#actually abused#Amber heard#actuallyabused#actuallytraumatized
24 notes
·
View notes
Text
I NEEDED THAT WORD!

Michael Schneider
62K notes
·
View notes
Note
Hope this isn't offensive (feel free to ignore if it is) but what illnesses do you have? I always see very detailed posts from you about different types of hyperspecific injuries or illnesses and I was wondering if you're just super well informed or have all of them.
Which is very helpful and cool for people who need the info, and I'm sorry if you are experiencing all those.
Oh, Christ. Right this is going to be a lot 😅
Conditions I have been diagnosed with as of 2024:
Ehlers Danlos Syndrome
Mast Cell Activation Syndrome
Dysautonomia/POTS/autonomic failure (they all mean a similar thing. I just have them all listed in my file because no one can decide what I actually have beyond “nervous system broke”)
Chronic Migraines
Hemiplegic Migraines
Cluster Headaches
Cranial Instability (caused by my EDS + neck injuries)
Trigeminal neuralgia
Occipital Neuralgia (caused by the cranial instability)
Binocular Vision Disorder
PMDD (likely linked to the MCAS)
Probably endometriosis but it’s unconfirmed.
Interstitial cystitis (definitely caused by the MCAS)
GERD (a symptom of my MCAS)
Pernicious Anemia (likely linked to the EDS and MCAS. I don’t absorb nutrients from my food as well as I should which is common when MCAS damages the GI tract.) which lead to hemolytic anemia in 2019 aka the “Almost Died For Real” year.
ADHD.
cPTSD
Dysthymia or “double depression”
“Probable ME/CFS” is in my file, but with everything else going on chronic and debilitating fatigue is pretty much unavoidable so my doctors are like 🤷🤷♀️
I had an intestinal perforation a few years ago that lead to severe diverticulitis that took about a year and a half to heal, but that’s healed now save for the occasional bout of nerve pain.
Uuuh… I think that’s it… (wait and see my spouse/friends chiming in with “you forgot about x”)
So yeah.
Chances are if you see me talking about it, I have it. I do sometimes talk about other conditions that I’ve learned about over the years of navigating my own stuff, but I will always defer to the lived experiences of others when it comes to their own conditions.
It’s a lot to deal with. Most of it links back to the MCAS/EDS/Autonomic failure.
Or as we like to call it: the generic trifecta of bullshit.
2K notes
·
View notes