#Quitsmoking
Explore tagged Tumblr posts
Text
🌱 Tobacco Harm Reduction: Pakistan’s New Hope to Stop Smoking!
Pakistan faces a smoking crisis with millions affected and rising healthcare costs. Traditional anti-smoking methods, like high taxes, only push smokers towards unregulated products, increasing health risks.
But there’s a better way—Tobacco Harm Reduction (THR). By embracing safer alternatives like vapes and nicotine pouches, Pakistan can make strides toward a healthier future.
Let’s spread the word and support THR as a vital part of Pakistan’s health strategy! 🛡️
#TobaccoHarmReduction #StopSmoking #Pakistan #PublicHealth #Vaping #NicotinePouches #QuitSmoking #HealthyChoices #Awareness
7 notes
·
View notes
Text
QUITTING IS WINNING
Let's all be quitters today!! I've been here before but this will be my last time. I desperately need to stop smoking weed.
Why am I quitting?
I want to respect myself again. I want to look in the mirror and not want to cringe. I want to see myself as worthy.
To save my life. I have no job at the moment and smoking isn't helping me find one.
To save my marriage. I'm not actually interested in my husband when I'm high.
We can do this.
4 notes
·
View notes
Text
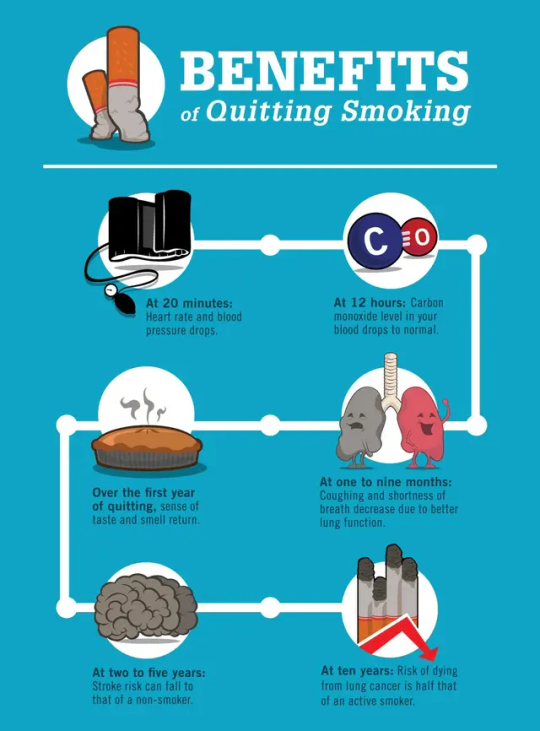
Smoking is a top global polluter whose pollution production contributes to climate change (n.d.). Smoking is an addiction that affects emotional and physical health. The physical addiction to smoking can be traced to nicotine in each cigarette (Siegel, 2022). Vaping, tobacco, cannabis, marihuana, and other illegal drugs are considered to be a form of smoking.
Vaping affects the environment differently by generating an extremely high volume of waste (Prochaska & Velicer, 1997). Nevertheless, there is a misconception that vaping can be an alternative option to quit smoking. However, vaping is no different than smoking tobacco. That misconception led to an increase in the pandemic of vaping, which attracts the youth to flavored vapes (n.d.).
“Smoking is both physical and psychological addiction, but quitting smoking can be done. The Centers for Disease Control and Prevention (CDC), 2018 estimated that 55.1 percent of adult smokers in the United States gave up the habit for more than one day to quit. Since 2002, the CDC reports that the number of former smokers has remained greater than that of current smokers in the United States.” (Siegel, 2022).
The social environment influences smoking, and psychologists can assist with alternative behavioral changes to help individuals who want to quit smoking (Van de Brand, 2019). Quitting smoking can be challenging and impactful on physical health and emotional changes. The nicotine in cigarettes and the act of smoking harvest a calming effect of mental clarity and relaxation that is perceived as a social activity and as a coping mechanism (Centers for Disease Control and Prevention (CDC) (n.d.). However, smoking has the opposite effect than what is believed. It increases anxiety level tension, and over time, smokers are more likely to suffer from depression secondary to smoking, health disease, emphysema, lung cancer, as well as other medical conditions secondary to smoking. Regardless of whether it is cigarettes, vaping, or e-cigarettes, an option used mainly by young adults and teenagers is a habit that can cause lifetime health damage.
Therapeutic Approach
Smoking cessation group therapy’s objective is for smokers to learn vicariously from their peers in group sessions to quit together to motivate and stimulate each other through peer pressure to improve the quit success rate and participation in the group (Van de Brand, 2019).
Smoking cessation therapy emphasizes techniques and mechanisms to quit smoking. To date, at least 40 evaluated anti-smoking programs or campaigns. Nine programs/campaigns were motivational informational, 11 were promotion specifics cessation activities, and 20 were mass media cessation “self-help clinics” (DPhill,1987). The CDC resources for quitting are in many languages. For the purpose of this assignment, I will only provide the Spanish and English telephone numbers. There are text message services and Smartphone apps, Tips, information, and challenges to help smokers quit.
Begin your journey today! Quit Smoking today!
Resource for Quitting 1-800-QUIT-NOW (1-800-784-8669) English
1-855-DÉJELO-YA (1-855-335-569) Español
Evaluation of the Ethnic Inequalities
The evaluation is not one of ethnic inequality but one of gender inequity between men and women smokers and non-smokers. Smoking rates are higher among couples who are married or living with a partner, social isolation, socioeconomic status, and isolation (Martin et al., 2019). Research suggests that marital status or living with a partner leads to a high likelihood of quitting smoking, and having a non-smoking partner increases the possibility of quitting smoking (Martin et al., 2019).
Mass Media Programs and Campaigns Designed to Reduce Smoking Behavior.
Mass media is a significant influencer in the increase and awareness of the danger of smoking, motivating smokers to quit and helping many ex-smokers to quit successfully.
The CDC spearheaded a campaign named “TIPs” to address the health disparities in smoking cessation to bridge the gap of health equity, representation, accessibility of smoking cessation programs, and assistance for smokers who are receptive to quitting smoking regardless of income, geographic location, or who they are.
The objective of the “TIPs” campaign is to increase the awareness of free smoking cessation educational resources among adults- adults- no matter who they are, where they live, or how much money they make (CDC, n.d.).
The “TIPs” campaign places a variety of tips ads in the media channels, reaching out to the community and groups with high levels of smoking-related disease management, including those populations that are disproportionally affected by tobacco use (CDC, n.d.).
The social influence attached to this research in the UK suggests that having a partner who quits smoking has a more significant impact on smoking tobacco than having a non-smoker partner (Martin et al., 2019). The workplace also favors smoking cessation, where colleagues are strongly associated with quitting success (Van de Brand, 2019).
Martin et al., 2019 report the social gradient to quit smoking on socioeconomic status in women is lower and may be less successful for men in quitting and women who had nonsmoking partners compared to women who had a partner who smokes at both points, having a partner who was non-smoker throughout was associated with a doubling of the odds of stopping smoking 99% and having a partner who smoked initially but stopped in the next four years was associated with 6 -fold increase in odds of quitting smoking 99% (Martin et al., 2019). Smoking cessation is highly associated with the workplace setting supporting smoking cessation and is strongly associated with quitting success (Van de Brand, 2019). Therefore, it is proposed that social change does influence smoking and smoking cessation.
The Role and Responsibilities of Psychology Concerning Smoking Cessation.
Psychologists have been advocates for smoking cessation throughout the years. Psychologist advocacy by APA not only gets reimbursed for being in the lineup of providing screening, smoking cessation treatments, and brief interventions for tobacco use. Action for compensation for therapeutic services, coverage for treatments, substance abuse, adopting smoke-free policies in public settings, and anti-smoking educational campaigns have been taken. Evidence-based information reflects a decrease in the use of cigarettes at the same time, contributing to the decline in smoking nationwide rates, reflecting the progress in services to help people during the challenges to quit smoking (Novotney, 2022).
Steps were taken to incorporate psychological treatments to intervene with patients’ smoking cessation therapies into existing behavioral health treatments to assist smokers with depression, anxiety, or other mental health conditions (Novotney, 2022). It would be conducive to the success of the smoking cessation regimens. Wilson Compton, MD, deputy director of the National Institute on Drug Abuse (NIDA), reports the long-term effects of smoking cessation would lead to a healthier lifestyle for “all people” when healthcare providers take a holistic approach to health issues and patient experiences, substance abuse disorders, and mental health disorders. Novotney (2022) goes on to say with the continuity of smoking; smokers can develop depression consequently to smoking. Therefore providing assistance and skills to quit smoking is essential in any platform. whether it is at work, school, clinical setting, or everyday interactions.
Because of the addictive concerns of smoking as a mental health condition and the withdrawal symptoms as any drug dependency, the withdrawal symptoms are comparable to cocaine and heroin, resulting in craving, anxiety, agitation, nausea, depression, and dizziness (Siegel, 2022). The dependency on nicotine makes it challenging to quit smoking, whether it is cigarettes, e-cigarettes, or other tobacco products. Nevertheless, psychological treatments and critical strategies can influence behavioral changes with tools for smoking cessation.
Social Changes /Social Justice.
The theoretical framework that would shape the behavior of my social change would be the transtheoretical model or the stages of change model. This model helps navigate to understand why people “stop smoking” and “how to do it .”The transtheoretical model suggests that health behavior changes involve a process through six stages of change (Prochaska & Velicer, 1997). The transtheoretical model can help smokers move through a series of phases before they quit smoking successfully. The change cycle is a phase one goes through when implementing behavioral change. Pre-contemplation (no plans of stopping), contemplation (planning on quitting), and preparation (planning to quit within the time next 30 days) (Prochaska & Velicer, 1997). Are the steps followed or experienced before making a lifestyle change?
In preparation for changes, access to mental health care can bridge the gap between the challenges and social changes in addressing the long-term effects of smoking, motivating and helping clients to quit smoking. Promoting health education and encouraging therapeutic intervention open the doors and facilitate the process of adaptation to quit smoking.
Addressing environmental factors, research findings on the effects of nicotine, triggers, preparation, and counseling can stimulate successful smoking cessation. Consequently, it leads to better health outcomes, identifying a plethora of reasonable motivators and products of smoking support. The assistance of “Physicians, regulators, and educators should discourage youth and everyone from attempting to use e-cigarettes as a way to stop smoking.” (PsycInfo Database Record (c) 2023 APA, all rights reserved).
Since better health insurance coverage for smoking cessation, developing new addiction treatment has been advocated by psychologists. The decline in smoking among adults, from 20.9% in 2005 to 12.5% in 2020, according to research by the U.S. Center for Disease Control and Prevention, has been noticeable (Novotney, 2022). Patient education should include community outreach, Public Announcements (PSAs), educational flyers, one-on-one patient education appointments with a smoking cessation wellness coach, psychological treatment, medical intervention, free smoking cessation medications, and no referrals required for smoking cessation counseling from primary care providers. These are great incentives, motivational tools, and resources to stop smoking.
The mentioned suggestions are important segway in exploring the methods and new perspectives to focus on adapting to changes through environmental factors, research findings, and the validity of outcomes on information, strategies, and accessible instruments as interventions for smoking cessation. At the same time, it emphasizes triggers, life experiences, practices, and beliefs that lead to smoking and vaping becoming a gateway to other drugs.
Educating smokers about resources available in the community, hospitals and mental health services, and helplines for smoking cessation are valuable tools for successfully quitting smoking.
Promoting Outreach programs in the community, mass media, reputable sources, and schools where kids are vaping flavorful e-cigarettes and vaping pens, all appealing to the younger generation by providing misleading information on TV, social media, and mass media that vaping is not as harmful as tobacco. In 2019, California researchers did some “shoe-leather investigating.” They discovered that by collecting tobacco, cannabis, and vape waste from a dozen high school parking lots across the San Francisco Bay Area, vape waste made up 19% of the litter recovered, let alone other pollutants from environmental vape (California Department of Public Health End Tobacco Damage Now, n.d.).
Therefore, parents, educators, school psychologists, school nurses, mental health professionals, and other community service programs need to educate the public on the long-term effects of smoking, e-cigarettes, vaping, tobacco, marijuana, and other smoking products effects on mental health and physical health. That will otherwise create a pandemic, and increasing dependence on smoking will become a mental health and physical public health burden that will be difficult to maneuver into incorporating behavioral change modification in the pursuit of promoting smoking cessation.
Subsequently, the goal is to incorporate psychological treatment where clients feel safe to thrive, with interventions and smoking cessation therapy, into existing behavioral health regimens for smokers with depression and any other mental health disorder or behavioral condition (Novotney, 2022).
Given the approval of the APA for secure reimbursement for psychological treatment and billing for psychotherapy services for smoking cessation. This approach will allow patients to receive care on a one-on-one basis or in a group setting for smoking cessation, including motivational interview-based interventions instead of physicians providing the treatment when psychologists are the ones who train physicians on motivational interviews and behavioral change modification.
Reference
California Department of Public Health (n.d.). End Tobacco Damage Now.
Center for Disease Control and Prevention (CDC) (n.d.). Tips From Former Smokers.https://www.cdc.gov/tobacco/campaign/tips/index.html
DPhill; B. R. (1987). Mass Media and Smoking Cessation: A Critical Review. American Journal of Public Health.77 (2).
HOPE TMS AND NEWUROPSYCHIATRIC CENTER (n.d.). How Can a Psychologist Help with Smoking Cessation (n.d.).
Martin; J. L., Barnes; I, Green; J, Reeves, G. K., Beral; V, Floud, S. (2019). Social Influences on Smoking Cessation in Mid-life: Prospective Cohort of UK Women. PLoS One. 14 (12):
Novotney; A (2022). American Psychological Association. APA Advocates for Psychologists Working to Help Patients Stop Smoking. 53 (7) pp. 26.
Prochaska, J. O; DiClemente, C. C; Velicer, W. F; Joseph S. Rossi; S. J. (1993). Standardized, Individualized, Interactive, and Personalized Self-Help Programs for Smoking Cessation. Health Psychology. 12 (5) pp. 399-405. The American Psychological Association, Inc., and the Division of Health Psychology/0278-6133/93
Prochaska; J. O, Velicer; W.F. (1997). The Transtheoretical Model of Health Behavior Change-American Journal of Health Promotion: AJHP, 12(1), 38-48. doi:10.4278/0890-1171-12.1.38. https://pubmed.ncbi.nlm.nih.gov
Pollution from Production to “Disposal”: The Life Cycle of Vape (2023). Environmental Destruction.
Siegel; J. (2022). Smoking Cessation. Salem Press Encyclopedia of Health. e0226019. doi: 10.1371/journal.pone.0226019
Van de Brand; F, Nagtzaam; P, Nagelhout; D. G, Winkers; B, Van Schayck; P. C. (2019). The Association of Peer Smoking Behavior and Social Support with Quit Succes in Employees Who Participated in a Smoking Cessation Intervention at the Workplace. International Journal Enviro Research and Public Health. 16 (16):2831 doi: 10.3390/ijerph161281 https://www.ncbi.nim.nih.gov
2 notes
·
View notes
Text

Smoking is just a gateway to all types of Cancer and a major reason for 13 types of Cancer and that’s not a enough reason to quit it.
#smoke#enjoysmoking#lovesmoking#tobacco#smokingkills#health#healthcoach#quitsmoking#smokebomb#smokeyeye#usa#florida#miami#newyork#giveupsmoking#unitedstates#universitycancercenter#cancel#floridalife
3 notes
·
View notes
Text
youtube
Quit Smoking, and after your last cigarette, THIS HAPPENS TO YOUR BODY.
Douglas Vandergraph continues his journey of teaching others how to accomplish their dreams and goals by explaining the timeline of health benefits that may occur in your body after you quit smoking. This discussion involves the believed timeline of health benefits that occur almost immediately after your last cigarette. Douglas is putting himself out there as an example to others so they can see how anyone can take a chance, improve daily, and make a difference in the lives of others. What is it that you want in your life? Douglas can show you how to get it! This is a video series Douglas is completing in the hopes he can help just one person. Dr. Suess once said, "To the world, you may be one person, but to one person, you may be the world."
Low Cost Online Resources to help you with addiction:
BETTERRHELP:
https://www.betterhelp.com/get-started/
TALKSPACE:
https://try.talkspace.com
ONLINETHERAPY:
https://www.online-therapy.com
Follow Douglas on Youtube:
https://www.youtube.com/@douglasvandergraph
Relevant Keywords:
#quitsmokingnow #quitsmoking #quitsmokingtoday #whathappensafterIquitsmoking #cigarettes #cigarette
#quitsmoking#cigarette#cigarettes#youtube#motivation#success#success story#successful#successstories#motivationalspeaker#motivationalstory#inspirationalstory#motivateyourself
2 notes
·
View notes
Text

Dit noemt men 'derdehandsrook'. Dit is de rook die achterblijft in kleren, in de auto of in het bankstel. Rook die ergens intrekt kan daar maanden blijven hangen.
Wees een held, redt jouw bankstel!
Lees meer:
https://www.ikstopnu.nl/bibliotheek/meeroken-en-derdehands-rook/#wat-is-derdehands-rook
#stoppenmetroken #stopsmoking #nogarette #quitsmoking #stopsmokingnow #stoptabac #stopsmokingcigarettes #stoptabak #rookvrij #rookvrijegeneratie #roken #stoproken #smokefree #healthylifestyle #smoking #quitsmokingtoday #weetje #funfact #fact #schadelijk #stof #stoffen #sigaret #huis #home #hecht #derdehandsrook #thirdhandsmoke #kleren #clothes #auto #car #bank #maanden #months
https://www.nogarette.com
#nogarette#quitsmoking#stoppenmetroken#stopsmokingcigarettes#stoptabac#stoptabak#no-garette stoppen met roken#stop smoking#no-garette stop smoking#stop now#facts#fun facts#interesting facts#cars#autos#bank#sofa#clothes#secondhand smoke#smoke#thirdhand smoke
2 notes
·
View notes
Photo

PSA - Quit Smoking
Designed by Slohand, t-shirts and more available at Redbubble
https://www.redbubble.com/people/Slohand/shop?asc=u&ref=account-nav-dropdown
4 notes
·
View notes
Text

गुटखा खाकर, पान चबाकर नहीं बढ़ेगा सम्मान, इसलिए आज से रखो अपनी सेहत का ध्यान।
#jaipurmensclinic#notobacco#stopsmoking#quitsmoking#smokingkills#nosmoking#worldnotobaccoday#health#saynototobacco#smoking#vape#vaping#smokefree#cigarette#notobaccoday#smoke#tobaccofree#nosmoke#motivation#vapeshop#tobacco#cbd#covid#vapelife#stopsmokingstartvaping#hemp#vapeon#vapers#vapenation#vapecommunity
2 notes
·
View notes
Photo
“You are not living if you are smoking….. you are taking small steps towards a disastrous life….. Say no to smoking and tobacco to live a healthier and happier life.” WORLD NO TOBACCO DAY 2023
#notobaccoday#notobacco#worldnotobaccoday#quitsmoking#smokingkills#quitsmokingtoday#nosmoking#tobacco#smoking#stopsmoking#quittobacco#healthylifestyle#tobaccokills
2 notes
·
View notes
Photo

Tobacco does not only harm the smoker – it also harms the producer. “We need food, not tobacco” campaign raises awareness about alternative crop production for tobacco farmers and encourages them to grow sustainable, nutritious crops. #NoTobacco #TobaccoExposed @uicc @who
#WorldNoTobaccoDay#WNTD2023#WorldHealthOrganization#QuitSmoking#StopSmoking#GrowFoodNotTobacco#FoodNotTobacco#NoSmokingDay#SayNotoCigarettes#Tobaccokills#MomentMarketing#Creativespot#MarketingAgency#DigitalMarketing#BrandingAgency#DigitalMarketingAgency#AdAgency#CreativeAgency#BCCUNITED
3 notes
·
View notes
Text

Quit Smoking Fast – Naturally!
🔥 NOW BUY 1 GET 1 FREE
Quit Smoking with Premium Organic Hemp Cigarettes (Hempettes) – Now at CBD+ Health Boutique of Deerfield Beach! 🌿
Looking to quit smoking without the harsh withdrawal symptoms? Discover the natural way to a healthier lifestyle with our Premium Organic Hemp Cigarettes (Hempettes) – now with an irresistible Buy 1 Get 1 Free offer at CBD+ Health Boutique of Deerfield Beach!
🌱 Why Choose Our Hempettes? Our hemp cigarettes are carefully crafted using:
- Premium Organic Hemp - Organic Mullein – known for its lung-supporting properties - Organic Sage – calming and aromatic for a smoother experience - Zero Nicotine
These ingredients work together to naturally reduce cravings, giving your body and mind the support they need to break free from tobacco addiction.
🚭 Quit Smoking the Natural Way Whether you're transitioning away from nicotine or simply want a cleaner smoke alternative, our Hempettes offer a satisfying experience without the harmful chemicals found in traditional cigarettes. No additives, no nicotine, no regrets.
💚 A Healthier You Starts Here Choosing plant-based alternatives like hemp, mullein, and sage can:
Promote better respiratory health Help curb nicotine dependency Support overall wellness
Align with a more mindful, holistic lifestyle
📍 Visit Us Today in Deerfield Beach! Come into CBD+ Health Boutique of Deerfield Beach to grab your Buy 1 Get 1 Free pack of Hempettes and take the first step toward a healthier you. Our knowledgeable team is here to guide you and answer all your wellness questions.
🕒 Store Hours: 11--7 PM 📍 145 E Hillsboro Blvd, Deerfield Beach, FL 📞 Call us at (954) 531-4782 🌐 Visit: vitaminy.com
#cbdplushealthboutique#cbd#cbdforpain#cbdoil#cbdoilnearme#cbdforanxiety#deerfieldbeach#cbdstore#cbdforpets#cbdindeerfield#quitsmoking
0 notes
Text
**Quit Smoking Hypnosis**
Break free from cigarettes with **Quit Smoking Hypnosis** at UniqueLy Northern. Our powerful, proven method helps reprogram your subconscious mind to eliminate nicotine cravings and change your habits for good. Instead of relying on willpower alone, hypnosis targets the emotional and psychological patterns behind smoking. In just a few sessions, clients often feel empowered, calm, and in control—without the usual stress or withdrawal. Say goodbye to smoking and hello to a healthier, smoke-free life today.
#QuitSmoking#HypnotherapyToQuitSmoking#UniqueLyNorthern#SmokeFreeLife#HypnosisHealing#FreedomFromSmoking
0 notes
Text


Discover Klyft – a clean, modern alternative to traditional nicotine. Smoke-free, mess-free, and designed for your lifestyle. Elevate your nicotine experience today.
#NicotinePouches#SmokeFree#NicotineAlternative#Klyft#QuitSmoking#NicotineLifestyle#TobaccoFree#ModernNicotine#HealthyHabits#VapeAlternative#MinimalDesign#CleanLiving#NicotineProducts#WellnessChoices#Smokeless
0 notes
Text
youtube
In this video, Dr. Komal Chaudhary, Consultant Pulmonologist at Mukat Hospital & Heart Institute, provides valuable tips to help you maintain healthy lungs and enhance your respiratory well-being. Whether you're managing seasonal allergies, coping with air pollution, or aiming to improve your breathing, these expert insights will support you on the path to stronger lungs and better overall health.
#HealthyLungs#LungCare#Pulmonology#BreatheBetter#DrKomalChaudhary#MukatHospital#RespiratoryHealth#HealthTips#QuitSmoking#AirPollution#LungHealth#Youtube
1 note
·
View note
Text

You are not sharing for happiness, you are manifesting ending together.
.
.
Visit : https://www.gr8brews.com/
#advertising#branding#marketing#digital marketing#360marketing#gr8brews#social media marketing agency#brands#creativity#trending#no smoking#smokefreelife#breatheeasy#worldnosmokingday#quitsmoking#healthfirst
0 notes
Text

31/5/2023
Vandaag is het Wereld Niet Roken Dag! 🚭
Een internationale dag waarop vele rokers in ieder geval één dag niet roken!
Ieder jaar staan wij alle stil staan bij de schade die roken wereldwijd aanricht.
Vorig jaar werd er aandacht gevraagd voor de onnodige schade die de tabaksindustrie aan het milieu aanbrengt en de meer dan 8 miljoenen jaarlijkse veroorzaakte doden.
Dit jaar staat de dag in het teken van de meer dan 5 miljoen voetbalvelden aan tabaksplantages die de ruimte van de voedselvoorziening innemen en de grond uitputten.
"We need food, not tobacco."
Stop 1 dag met roken voor de gezondheid van jijzelf en de aarde.
Doe jij ook mee?
Zeg Nee, tegen de sigaret. Samen met No-Garette!
Stoppen met roken?
www.NoGarette.nl
🍀

#wereldnietrokendag#worldnotobaccoday#growfoodnottobacco#weneedfoodnottobacco#stoppenmetroken#quitsmoking#31mei#31may#nogarette#stopsmokingnow#stopsmokingcigarettes#stoptabac#stoptabak
4 notes
·
View notes