Text
Over the last two weeks, we’ve rotated through three new clinical sites, each representing a different level of care. Mount Meru Regional, where we spent our first two weeks, is the highest level of care. Tengeru District Hospital, our next stop, is a smaller district center with less resources and fewer departments. There, I spent my time in pediatrics. It was a more relaxed experience, as patient acuity was lower, however, significantly less intellectually stimulating. I would venture to say that 90% of the kids we say were being hospitalized for an upper respiratory infection or pneumonia. My three biggest takeaways:
The sick, sick kids are at Mount Meru Regional.
They prescribe antibiotics for every cough + fever, virus or not.
There’s no concern about antibiotic resistance even though I’ve only seen a handful of abx used.


Next, we spent three days at a local health center, the next level of care, and two days at a dispensary, the lowest tier. At the health center, there was only outpatient, reproductive health, pharmacy, and laboratory. I saw my first patient present with acute Malaria! Unrelated, but here’s an entertaining infographic on Ebola:

This last week, we’ve returned to the ER at Mount Meru Regional Hospital. We’re done being shy because intern doctors, with similar level of education to us, are running the department. They're preforming the same procedures that we’ve been trained for, making mistakes that we can help address with fresh eyes, and they’re willing to work with us like we’re colleagues. So we dive in.
Woman presents convulsing, one week postpartum. Eclampsia. She can’t maintain her own airway, but they do not intubate. Admit for observation, but she’ll likely never walk out of this hospital.
MVA. Grossly disfigured humoral fracture and dislocation. Scalp flap and large lower leg laceration. Diclofenac and local lidocaine only for pain control. He’ll be seen for surgery in two days.
Machete attack to the neck, hand and back. Common here. Hours worth of suturing. He’ll survive. Another machete attack survivor, pictured here (photo courtesy of Kate Varano).

A paraplegic woman (due to a hemispheric hemorrhagic stroke four years prior) presents with a possible new CVA. Her high fever and questionable vitals indicate that she’s also septic, whether the source is her turbid urine or the course crackles throughout bilateral lung fields, I’m not sure. Oh, and she’s a Type 2 Diabetic, so she’s also in HHS (hyperosmolar hyperglycemic state). Kussmaul breathing, clearly acidotic. GCS of 4. She needs to be intubated, but that’s not a consideration here because the entire hospital has only one vent. I’m not sure if it’s ever used. Interestingly enough, she would likely be a DNR patient in The States. But, despite the many patients I’ve seen treated with minimal intervention- the doctor is ordering at 250,000 TSH head CT that her husband will pay for, despite the unfortunate fact that the results will not change management nor improve prognosis.
Active TB patient with unilateral leg swelling, tachycardia, and difficulty breathing. Probable PE. Desaturating as we speak. Will be admitted for observation.
Another active TB patient, older Maasai woman with end stage AIDS, cryptococcal meningitis, coughing up copious amounts of blood. Drowning in her own blood, essentially, while we perform oral suction and watch her oxygen saturation plummet and her heart rate soar. Again, intubation is not considered despite our pleas. We wait expectantly for her heart to arrest. Miraculously, after what seemed like hours, the bleed must have clotted off. Her saturation rises to 92% and we admit her.
Noah, a fourteen year old Maasai boy who speaks only his tribal dialect and looks like he’s closer to eight years old. His dad is at his side, which is rare for pediatric patients. They’re both terrified and no one speaks a language that they can understand. The limited history we receive illustrates a cardiac anomaly at birth (no evidence on physical exam) nephrotic syndrome, and liver disease secondary to herbal medicine. He’s in respiratory distress, heart rate + blood pressure are holding stable for the time being, but his extremities are as cold as a corpse. He’s the picture of extreme septic shock. He’s grunting to breathe and manages to communicate simply “I’m tired”.
I could continue to log interesting patients for the rest of this blog post, but I can’t stop thinking about Noah. So I’m going to talk about him.
My heart shattered yesterday, not because of the limits of medicine, resources or physician competency here. That’s hard, but that’s what I’ve been coming to terms with for the last five weeks. I can wrap my mind around that. What I can’t wrap my mind around is the lack of humanity. All I could think about, while I squeeze Noah’s hand, is being hospitalized myself. The compassion and respect I was treated with. I try to mirror the empathy that I was treated with, that made my hospitalization more bearable and less terrifying/isolating/dehumanizing, for my patients. With Noah, no one spoke to him. Not while poking and prodding, not while collecting blood or urine samples, not while he gasped for breath and communicated his terror with his eyes. No one attempted to communicate with his father because they don’t speak his language. But fear is a universal language. As is compassion. I did all that I could; simply acknowledge the fear in their eyes and return their gaze with empathy and care in mine. And it wasn’t even close to enough.

He’s in the pediatric ICU now. He’s not doing well. Hanging on, though.
And I’m going to hang on to the smile I got out of him while I held his head and apologized, in broken Swahili, for being a white girl who only knows English.
0 notes
Text
911
Week Two: 🚑
My heart needed a break from dying babies and feeling helpless, so I decided to spend my second week in the emergency department, hoping this is somewhere I could actually be of use. Unfortunately, I think my heart is heavier still after this week. On Monday morning, within minutes of stepping into the ward, I passed a hallway with a single gurney that held a small body, covered completely by a Maasai cloth drape. The paper laying atop the body read simply:
Age: 5
Gender: Female
Cause of Death: Unknown.
I stepped into the bathroom to catch my breath.
Our first patient, a 60-ish year old male, presented with a blood-filled mouth, left sided hypertonia, right sided facial drop + hyperactive hand movement. It costs 12,000 TSH to be seen by a doctor. His coworkers, who transported him to the ER, had to pay before he was allowed in the doors. Point of care testing for HIV was immediately preformed: negative. They don’t have the ability to order a drug/tox screen. The next step, after collecting a limited history, was a head CT, but that costs 250,000 TSH (which is approximately three months salary for the patient). For hours, as the patient continues to respond minimally, the coworkers call friends and family members to see if they can put together enough money to pay for the CT scan. They finally conclude that it won’t be possible, but they can pay the 12,000 TSH it costs to be admitted for the week for observation. (Trauma Bay pictured below)
A plethora of unique patients roll in, one after another after another after another. None of them speak any English, making clinical investigation and management a slow and tedious process. Each patient seems more critical than the next. Unlike the United States, where most patients present when an affliction becomes noticeable and/or bothersome, patients here wait to present to the hospital until it’s the only choice they have. This is especially true in the urgent care setting, where I saw, most notably, esophageal cancer so advanced the patient could barely swallow water and Non-Hodgkins lymphoma present with a mediastinal tumor the size of a small grapefruit that had been symptomatic for over a year. The MD that I was with let out a big sigh and said, “I hate giving bad news like this because in all likelihood, she won’t be able to pay for treatment.” Making this a terminal diagnosis, even though it wouldn’t need to be in the States. This hit me like a lead pipe against the head: I would almost certainly be dead if I lived here at the time of my cancer diagnosis.
Thursday met us with perhaps the most gut wrenching patient yet. An 8 year old boy was brought in by his family, who discovered him convulsing when they went to wake him that morning. No real history could be ascertained. He appears dramatically malnourished. Pupils constricted but reactive to light, tachycardic with a mild fever noted, other vital signs normal. No nuchal rigidity. Blood sugar within normal limits. GCS of 7 (No verbal response, no eye opening, withdraws from pain). Diazepam 10mg IV push given. During the next few episodes of convulsions, his heart rate spikes to the 170s. No fluid has been initiated yet. It’s been at least 20 minutes now. Hospital personnel have started to sit down to chart, go check on other patients, take their break, etc. I’m frozen on the spot beside this child feeling sick to my stomach and helpless. It’s not my place, here, to interject my medical opinion. But, as I watch him start to seize again and his heart rate rise, I step out into the hallway and ask one of the intern doctors, “Should we start some fluid to decrease this heart rate?”. She responds, “Oh that’s a good idea!”, and returns a few minutes later with the equivalent of lactated ringers. When she returns to check on him 20-30 minutes later, he’s still convulsing. She decides to try Phenobarbital 100mg IV. Then another hour later, another 100mg IV. No change. They decide to admit him to the pediatric unit because they don’t know what else to do. Another patient comes into the trauma bay, so he’s taken off the monitor and left to await transport. Before he leaves the ED, I shine a light into his eyes and my fear is confirmed: pupils are pinpoint and fixed. Brain dead.

It’s infuriating, leaving the well-oiled machine that is emergency medicine in the States, and arriving to this. When a true emergency rolls through the doors at home, 15 people jump in, all with specific roles to fulfill. Everyone knows how dyer the situation is and we check every. single. thing. off the list of interventions to try before anyone even thinks of taking their eyes off the patient. We try and try and try and we don’t rest until the patient starts to improve or we know we’ve tried everything that we possibly can. Here, it seems as though death, even for children, is viewed as inevitable and it’s really not in our control whether it happens or doesn’t. I’m not sure if it’s because they don’t have the supplies or the equipment. I’m not sure if, because people seem to be dying left and right, they just don’t have the energy to fight what seems like another losing battle. I don’t know. What I do know is that this week I really struggled to understand the care and empathize with the providers here. Our program, and the general mission of global healthcare education, tells us that we’re supposed to be here to learn, not to teach (or preach), but I’ve never felt as hopeless and powerless as I did in that room, watching that little boy lose brain function by the second, minute, hour. It was a million times worse because I know other outcomes were possible.
And still, more patients roll in. Here’s my favorite from the day: a 40-something year old male in a motorcycle crash. Open comminuted femur fracture. He sat on a stretcher for HOURS in the ED awaiting surgery.
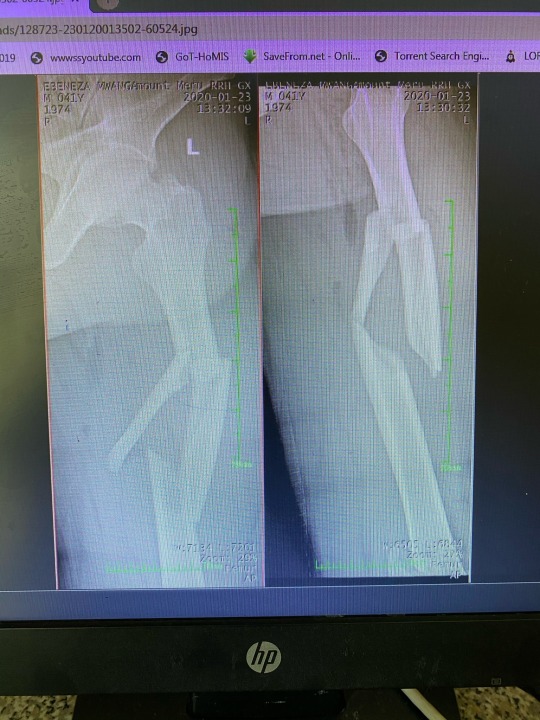

By the time Friday afternoon rolled around, I was mentally and emotionally exhausted and I needed a break. One very special kid, we’ll call him “J”, (he’s given me permission to post the following pictures) has been on the pediatric inpatient unit for the entire time that we’ve been here. Three weeks, stuck in bed with nothing to do except listen to the sick and crying younger children in neighboring beds. One of my classmates, Cienna, bonded with him from day one and discovered that he loves drawing. She brought him pencils and a sketch book and he asked to draw her earlier in the week. I happily volunteered to be next in line so by the time Friday afternoon rolled around, it was the most welcome way to recharge for me and, I hope, for J too. I sat in front of him making funny faces and getting to know him while he worked.

He told me when he grows up he wants to be an artist, and maybe a doctor too. His favorite subject in school, besides art, is science. He loves it when it rains and he has three older brothers. His mom died when he was younger, so it’s his aunt and uncle who sit vigil beside him, day in and day out. His uncle, John, a professional artist, calls J his star student. I know I’ll cherish my “J original” for as long as I live.


If you’re in the market for a beautiful art piece, John ships worldwide. I’ll attach his business card. Their art is such a ray of sunshine in this sometimes cruel world. Thank you both ❤️

0 notes
Text
We’re Not in Kansas Anymore
Our entire first week of this clinical rotation has passed and I’ve spent a lot of time thinking about what I should write about in this blog post. I’m still not entirely sure how to paint an accurate picture of everything we’ve seen and done here. I’m not typically at a loss for words either... We’re stationed at the largest hospital in the area, Mount Meru Regional Hospital, which hosts a bed capacity of 371 inpatient beds and recieves 200-300 outpatients per day.

I’ve been splitting my time between the neonatal ward + labor and delivery unit. If you’ve been witness to a hospitalized birth in the United States, you know that it is a meticulously monitored process. Before the mother steps foot into the maternity ward, she’s already subjected herself to months of pre-natal appointments, which undoubtedly included fetal heart tone checks, blood pressure monitoring + urine sample analysis, at the bare minimum. Here, pre-natal care is non-existent. Hospitalized births are reserved for the “privledged” and those with a complicated obstetric history. Mount Meru is a referral hospital, so many women are sent here from smaller, less equipped area hospitals. They average 400 vaginal deliveries and 200 cesarean surgeries PER MONTH. Mothers are herded from unit to unit depending on what stage of labor they’re in. When they are in active labor and greater than 7-8 cm dilated, they walk to the “delivery” room, which consists of 12 beds positioned less than two feet apart from one another. They labor together and give birth next to each other, surrounded by strangers, as no supportive family members are allowed in this room. It was less private than a blood donation drive in The States. Pictured below: (L): the corridor beyond the delivery room, where health babies are placed to wait while mom is sewn up (if need be) & cleaned. (R): a delivery bed.


In only a week, we witnessed and heard accounts of far too many stillbirths and maternal deaths. The fear that these women must have been feeling walking into this room, knowing that there is a high chance that she might not be walking out with her baby, or walking out at all; I cannot fathom. The youngest laboring mother we saw this week was only sixteen years old and she was crying for her mother in between pain filled screams.
Maternal death accounts for 18% of all deaths for women age 15-49. The three most common causes include preeclampsia, eclampsia, and post-partum hemorrhage.

And then there’s the babies. Oh, the babies. Each of them would be in an isolated incubator in the States, strictly limited from human touch and exposure to anything that could jeopardize their dangerously immature immune systems and underdeveloped lungs. Here, they lay in padded laundry baskets lined up beneath coil heaters mounted to the wall while flies swarm around the open air rooms.

They’re sorted in groups: ICU, sick, breastfeeding, deceased or sick mothers, and abandoned babies. They range in appearance from plump, happy babies to skeletal outlines that look like they’ll break if you move them wrong to 600g should-still-be-in-utero babies who, fun fact, haven’t even developed nipples yet. They’re considered “stable” and ready for discharge once they reach 1.5kg (3.3lbs).


They’re breast or bottle fed twice during our shift: 9:30am and 1:30pm. Mothers have to provide diapers, wipes, and breastmilk. Formula and hospital-provided supplies are strictly reserved for abandoned babies and babies with sick or deceased mothers. For premature babies, no steroids are given to assist in lung maturation. In fact, steroids have a terrible reputation here- in medical school, doctors are taught to steer away from their use entirely. For malnourished babies with hypoglycemia, 10% dextrose is administered regularly. And BG checks are repeated on a basis that depends on their current supply of test strips. Ampicillin + Gentamicin are the only antibiotics that I saw used, but they were employed generously. Oxygen is supplied through one portable machine, that outlets through tiny NG tubes that are inserted into the babe’s nostril. When multiple babies require oxygen, they are laid together so they can share the machine.

One baby, pictured below, who particularly tugged at my heart strings, came from home at 50 days old, presented severely malnourished with diarrhea and rectal prolapse. We found out that the mother had been supplementing her breastmilk with copious amounts of water and feeding him raw egg yolks when he cried at night, because that’s what another mother told her to do. The doctor told us that he’ll likely survive this hospitalization. Unfortunately, however, readmission rates are alarmingly high. Regardless of how much education they provide to mothers, often advice from other mothers will outweigh theirs, and most babies will return in decompensating, critical condition 2-3 more times before they ultimately succumb.

To say this week has been emotionally taxing would not do it justice. I am changed.
I have a newfound understanding of the bravery and strength it takes to become a mother here and the children who survive infancy? They have to be the most resilient humans I’ve ever laid eyes on. But most of all, I am in awe of the healthcare workers. With so few resources, so many heart wrenching stories and unfair deaths, they manage to impact the lives that they can and show up for work day after day to do it all again. 🏥🩺♥️
0 notes
Text
Polay, Mzumgu
Jambo & Happy New Year from the foothills of Mt. Kilimanjaro! 🏔✨

This is my first attempt at a blog, so bear with me. Aside from earning a sweet scholarship that MCPHS offers, my goal with this blog is to convince you to say “YES!” to an international rotation when the time comes. For now, however, read along with my journey:
My mom + I have been in Tanzania for nearly a week now, staying at the enchanting Kaliwa Lodge. We landed the after of December 30th, stayed up for a few hours socializing with the inn managers (a couple who uprooted from Germany a year ago!) and called it an early night so we could sleep off the jet lag + adjust to the 8 hour time difference.

Waking up refreshed on our first full day in Tanzania (which happened to be New Years Eve), we decided to venture out to Moshi, a local village bustling with excitement for the holiday. We visited a newly re-established train station & the local produce market, buying a bushel of bananas to snack on. It is notably warmer in the more “urban” areas than in the jungle, where the breeze and shade keeps you from ever feeling too hot. Culturally, there were a few quick adaptations that I made- Westerners are too direct here. Locals tend to beat around the bush/be more vague when asking and answering questions, directness can be viewed as rude. As can taking a picture of a large area (like the bustling market) with lots of people around. Additionally, it became quickly clear that in Tanzania, you eat what is available at the market that day. For this reason, the array of foods for meals can sometimes be limited to in season fruits and vegetables but the freshness is OUTSTANDING. I have spent the last 5 days eating my fill of the juiciest pineapples I’ve ever had, along with bruschetta on homemade bread, avocado salad, and fish or chicken with various fresh vegetables. It’s been heavenly. 🍌🍍🥑


Our New Years Eve celebration at Kaliwa lodge included a feast of local delicacies with travelors from Australia, Germany, Kenya, the US, France, and locals from six different Tanzanian tribes. We laughed, swapped stories, played games, and danced the night away. Josephine, one of the locals, explained as best she could in English, that NYE is so celebrated in Tanzania because it is a chance to remember all we have lost and those less fortunate than us and to celebrate all that we have; our blessings. Their excitement was contagious, it was one of the most magical nights of my life. 🌍

Over the past few days, we’ve been basking in the natural wonders Tanzania has to offer: waterfalls, river gorges + coffee plantations with our new friend Hilari, who spent all day teaching us about local history, traditions and day-to-day life in Machame, a small village situated at the base of Kilimanjaro.



We visited Kiwuletwa Hot Springs, somewhere I’ll undoubtedly return to in the rest of my time here. Crystal clear water flows here from the mountain and the sun warms it to a gloriously refreshing temperature. We were the first to arrive and spent the first hour or so swimming in the spring while dozens of monkeys swung from the tree canopy above. What an experience! 🐒

Yesterday, we spent our day at a a local animal rehabilitation center for misfits, injured or abandoned animals. Unlike in the states, where zoos are just tourist attractions for viewing caged animals- I’m happy to report that at this little known rehabilitation center, I saw animals treated better than my dogs at home (and they get pancakes on Sunday mornings so that’s saying something). Their owner, a veterinarian, has cast broken limbs of cheetahs and wings of owls, treated septic monkeys, amputated gangrenous appendages from dika and cerval cats, rehabilitated and adopted abandoned elephants, zebras, donkeys, sheep, goats, and horses. They’ve built a world for their animals where humans are the ones that have to enter cages to feed and care for them. Contact with humans aside from the care specialists is forbidden for some animals that they still hope to release back into the wild, but there’s a few that have made the sanctuary home: like Milay the monkey who really loved my blonde hair. 🦓🐆🦎🐘🦚🦉

Next week we embark on Safari + after that, the real work starts! I can’t wait to share this journey, come along for the ride!
1 note
·
View note