#Oral fluconazole
Explore tagged Tumblr posts
Text
Oropharyngeal primary syphilis by Dr Louis Noël in Journal of Clinical Case Reports Medical Images and Health Sciences
A 48-years-old healthy male was referred to our tertiary care center from an otorhinolaryngologist. The patient complained of odynophagia for the last 4 months, without any history of smoking nor chronic alcohol intake. A biopsy was performed and diagnosed chronic inflammation with fungal mycelia. Oral fluconazole did not bring any improvement.
Upon arrival, the examination shows some granular and erythematous pharyngeal lesions (Figure 1). A diagnostic work-up with local biopsies and serologies was done.
The PCR came back positive for Treponema pallidum (negative for herpes virus, chlamydia, and gonorrhea). Syphilis serologies were also positives (VDRL titer, 1:8; TPHA titer 20’480). The patient received one intra-muscular benzathine benzylpenicillin injection (2.4 million I.U.). The odynophagia and the lesions disappeared within 48 hours (Figure 2), without relapse for over two years.
Syphilis should be considered in every acute and chronic pharyngeal lesion, as oral sex may not be disclosed upon first medical consultation.
We declare no conflict of interest nor funding source. We obtained the patient’s written consent for the publication of this case report.
#Oropharyngeal primary syphilis#odynophagia#Oral fluconazole#jcrmhs#Journal of Clinical Case Reports Medical Images and Health Sciences submissions#Clinical decision making#Clinical Images journal
3 notes
·
View notes
Text
Cytochrome P450 Inducers & Inhibitors
The main ones can be remembered using "CRAP GPs spend all day on SICKFACES.COM".
Cytochrome P450 Inducers
These induce CYP450 activity, and thus reduce the concentration of drugs which are metabolised by this system.
Carbemazepine Rifampicin Alcohol (chronic use) Phenytoin Griseofulvin Phenobarbitone Sulphonylureas, St John's Wort, Smoking
Also topiramate.
Cytochrome P450 Inhibitors
These inhibit CYP450 enzyme activity and thus increase the concentration of drugs which are metabolised by this system.
Sodium valproate Isoniazid Cimetidine Ketoconazole Fluconazole Alcohol (acute use), Amiodarone, Allopurinol Chloramphenicol Erythromycin Sulfonamides, SSRIs Ciprofloxacin Omeprazole Metronidazole
Also grapefruit, cranberry juice, diltiazem, verapamil, clarithromycin.
Common Interactions
Medications which commonly interact with CYP450 inhibitors and inducers are:
Warfarin
Phenytoin
Combined Oral Contraceptive Pill (COCP)
Theophylline
Corticosteroids
Tricyclic antidepressants
Statins
Lamotrigine
Midazolam
#medical school#pharmacology#drug interactions#mnemonic#prescribing#med student#revision#cytochrome p450#cyp450#medicine#studyblr#medblr#warfarin
12 notes
·
View notes
Text
First-line therapy — Topical antifungal medications, topical selenium sulfide, and topical zinc pyrithione are effective and well-tolerated first-line therapies for tinea versicolor (table 1) [26].
Topical antifungals — Topical azole antifungals, topical terbinafine, and topical ciclopirox improve tinea versicolor via direct antifungal activity. Effective treatment regimens ranging from a few days to four weeks in length are reported in the literature [26]:
●Azole antifungals – Small randomized trials support the efficacy of various topical azole antifungals (table 2) [26]. In one randomized trial, ketoconazole 2% cream applied once daily for 11 to 22 days (mean 14 days) was superior to placebo (84 versus 22 percent achieved mycologic cure) [27]. A typical course of treatment with a topical azole antifungal is daily application for two weeks.
The shampoo formulation of ketoconazole appears to be effective with a shorter duration of therapy. The shampoo is applied to affected areas and is washed off after five minutes. In a randomized trial, a single application of ketoconazole 2% shampoo was compared with treatment on three consecutive days. Both regimens resulted in mycologic cure in approximately 80 percent of patients [28].
In accordance with the trial results, we consider both the three-day and one-day regimens for ketoconazole shampoo reasonable approaches to treatment. However, given the common location of tinea versicolor in skin sites that are difficult for patients to see and reach, the potential for environmental or patient-specific factors to influence the efficacy of treatment, and the minimal risks of treatment, we typically advise patients to treat for three consecutive days in an attempt to increase the likelihood of adequate treatment.
●Terbinafine – Topical terbinafine 1% solution applied twice daily for one week has been proven effective in small randomized trials [29,30].
●Ciclopirox – Topical ciclopirox olamine 1% cream was effective in two small randomized trials when applied twice daily for 14 days [31].
Selenium sulfide — Topical selenium sulfide exerts antifungal activity primarily through the promotion of shedding of the infected stratum corneum. In a randomized trial, application of selenium sulfide 2.5% lotion for 10 minutes for seven days was superior to placebo in achieving mycologic cure (81 versus 15 percent cured, respectively) [32].
The shampoo formulation of selenium sulfide 2.5% is often prescribed in clinical practice. Patients apply the shampoo to the affected area daily for one week. The shampoo is rinsed off after 10 minutes.
A non-prescription selenium sulfide 1% shampoo is also available, but the efficacy of this product for the treatment of tinea versicolor has not been studied.
Zinc pyrithione — In a controlled trial that included 40 patients with tinea versicolor, zinc pyrithione 1% shampoo applied for five minutes per day for two weeks was more effective than placebo for the treatment of tinea versicolor [33]. All patients treated with zinc pyrithione shampoo were successfully treated compared with none of the patients in the placebo group.
Severe or recalcitrant disease — Oral therapy is reserved for patients with tinea versicolor that is refractory to topical therapy or widespread disease that makes the application of topical drugs difficult [1,25]. It is important to note that persistent dyspigmentation is not a good indicator of failure of topical therapy. (See 'Treatment failure' below.)
Oral therapies — Oral azole antifungals such as itraconazole and fluconazole are effective for the treatment of tinea versicolor (table 1). In contrast to topical terbinafine, oral terbinafine is not effective [34]. Similarly, griseofulvin cannot be used for this condition.
Systemic therapy is not used as a first-line treatment for limited tinea versicolor to minimize risk of adverse effects. Abnormalities in liver function tests and drug interactions can occur with systemic azole antifungals. (See "Pharmacology of azoles", section on 'Adverse effects' and "Pharmacology of azoles", section on 'Drug interactions'.)
Oral therapy is not typically used for the treatment of tinea versicolor in children.
Itraconazole — Itraconazole therapy for tinea versicolor in adults is usually given as 200 mg per day for five days. Multiple randomized trials have reported mycologic cure rates between 70 and 100 percent with 200 mg of itraconazole daily for seven days, and dose comparison studies have shown similar success with treatment durations of five days [35].
Data conflict on the efficacy of a single 400 mg dose of itraconazole. In a randomized, open-label trial, a single 400 mg dose was as effective as 200 mg daily for seven days [36]. However, a low rate of response to a single 400 mg dose of itraconazole was reported in a trial that compared single-dose fluconazole and single-dose itraconazole [37].
Fluconazole — Fluconazole for tinea versicolor in adults is typically given as a 300 mg dose once weekly for two weeks [35]. In a small, uncontrolled study, 300 mg once weekly for two weeks led to mycologic and clinical cure in 75 percent of patients with tinea versicolor [38]. A dose-finding randomized trial also supports the efficacy of this regimen; 300 mg once weekly for up to two weeks resulted in mycologic cure in 87 percent of patients [39].
A single dose of fluconazole may be effective. In an uncontrolled study of 24 individuals with extensive or recurrent tinea versicolor treated with a single 400 mg dose of fluconazole, resolution of clinical disease occurred in 74 percent [40].
Other therapies — Additional topical and systemic therapies have been used for the treatment of tinea versicolor:
●Topical agents – Whitfield ointment [41,42] and sulfur-salicylic acid shampoo [43] are effective for tinea versicolor, but may cause skin irritation in a minority of patients. Small uncontrolled studies suggest that propylene glycol [44] and benzoyl peroxide [45] may also improve tinea versicolor.
●Oral ketoconazole – Although oral ketoconazole was effective for tinea versicolor in small randomized trials [46,47], life-threatening hepatotoxicity and adrenal insufficiency, along with multiple potential drug-drug interactions, have been reported with oral ketoconazole therapy, making it an unfavorable choice for the treatment of tinea versicolor. Although these adverse effects appear to be rare with the short duration of therapy used for tinea versicolor [48], knowledge of the potential for hepatotoxicity and the wide availability of safer oral antifungal agents led the European Medicines Agency to release a 2013 recommendation that marketing authorizations for oral ketoconazole be suspended throughout the European Union [49]. The US Food and Drug Administration (FDA) simultaneously removed its indication for use of the drug for dermatophyte and Candida infections based upon risks for hepatotoxicity, adrenal insufficiency, and drug-drug interactions. The FDA also recommended that oral ketoconazole should not be used as a first-line agent for any fungal infection. The indications for treatment of blastomycosis, coccidioidomycosis, histoplasmosis, chromomycosis, and paracoccidioidomycosis have been retained only for patients in whom other antifungal treatments have failed or are not tolerated [50]. (See "Pharmacology of azoles", section on 'Adverse effects'.)
In 2016, following an FDA safety review that found continued prescribing of oral ketoconazole for fungal skin and nail infections, the FDA released a drug safety communication warning healthcare professionals to avoid prescribing oral ketoconazole for fungal skin and nail infections [51]. The risks of oral ketoconazole treatment outweigh the benefits.
Treatment failure — Hypopigmentation and hyperpigmentation can persist for months following successful treatment of tinea versicolor, and may cause patients to assume incorrectly that treatment has failed. The presence of scale plus a positive potassium hydroxide (KOH) preparation is considered indicative of active infection.
Resistance to therapy, frequent recurrence, or widespread disease should prompt consideration of an immunodeficient state (table 3).
3 notes
·
View notes
Text
if you find that taking antibiotics usually gives you a yeast infection, you can ask your doctor to also prescribe fluconazole or another oral anti-fungal to prevent that, by the way...
Having a vagina honestly sucks bc it's like you have to do fucking alchemy just to prevent yourself from getting sick. You've got an intricate ecosystem of microorganisms down there that you're dependent on for your own well-being and they can be set off by the tiniest fucking thing
Keeping your pubes too short can cause yeast infections, but letting them get too long can also cause yeast infections. Washing the area with specialized soap can help prevent yeast infections, but it can also cause them. Your periods can cause yeast infections, and so can the medicine you take to stop your periods. Having sex can cause yeast infections, especially if the person you're having sex with is diabetic (???). Being diabetic can cause yeast infections. Wearing the wrong clothes or eating the wrong things can cause yeast infections. Not getting enough fucking sleep can cause yeast infections. The list is neverending
Luckily, yeast infections are fairly easy to treat with OTC medicine that you can find at any Walmart. BUT! Even if all of your symptoms indicate that you have a yeast infection, you have to take a test first to confirm that it's a yeast infection (they do not sell the tests at Walmart) bc you might actually have the opposite of a yeast infection (bacterial vaginosis) which has the exact same symptoms as a yeast infection but is caused by an imbalance of different microorganisms. And if you use yeast infection medicine to treat a bacterial infection it will light your pussy on fire. So if you have a bacterial infection, you must instead visit your local witch doctor (gynecologist) and get prescribed special potions (antibiotics) to treat it
Antibiotics can also cause yeast infections
59K notes
·
View notes
Text
Effective Solutions for Vaginal Infection Treatment in Thane

Vaginal infections are a prevalent health issue affecting women of all ages. These infections can cause discomfort, embarrassment, and serious complications if untreated. With advanced facilities and specialists like Dr. Aditi Godbole, women in Thane can now access exceptional vaginal infection treatment in thane, ensuring tailored care and effective solutions.
Understanding Vaginal Infections
Vaginal infections, or vaginitis, occur due to an imbalance in the vaginal ecosystem caused by bacterial overgrowth, fungal infections, or parasitic organisms. Common symptoms include itching, burning sensations, abnormal discharge, and unpleasant odors. Contributing factors include poor hygiene, hormonal changes, and certain products like scented soaps or douches.
Types of Vaginal Infections
Bacterial Vaginosis (BV): An overgrowth of harmful bacteria causes BV, leading to thin, grayish discharge with a fishy odor. While not sexually transmitted, it can be triggered by sexual activity.
Yeast Infections: Caused by Candida albicans, these result in thick, white discharge, intense itching, and swelling. Women with weakened immune systems or on antibiotics are more prone.
Trichomoniasis: A sexually transmitted infection caused by Trichomonas vaginalis, presenting yellow-green frothy discharge and discomfort during intercourse.
Non-Infectious Vaginitis: Allergic reactions to products like spermicides or detergents can cause irritation and inflammation.
Diagnosis of Vaginal Infections
Accurate diagnosis is essential for effective treatment. Dr. Aditi Godbole and other specialists in Thane employ comprehensive diagnostic methods, including:
Medical History: Assessing symptoms, lifestyle, and medical background.
Physical Examination: Conducting pelvic exams to detect inflammation, discharge, and abnormalities.
Laboratory Tests: Analyzing vaginal discharge samples to identify causative agents through microscopy or culture tests.
Treatment Options Available in Thane
Thane offers cutting-edge gynecological facilities with personalized treatment plans for vaginal infections. Key treatment options include:
Medications:
Antibiotics: Oral or topical antibiotics like metronidazole or clindamycin for bacterial infections.
Antifungal Agents: Creams, suppositories, or oral medications like fluconazole for yeast infections.
Antiparasitic Drugs: Metronidazole or tinidazole for trichomoniasis.
Lifestyle Modifications:
Avoiding scented products and harsh chemicals.
Maintaining hygiene and wearing breathable cotton underwear.
Practicing safe sex with protection.
Probiotic Supplements: Enhancing diet with probiotics to restore healthy vaginal flora and reduce recurrent infections.
Hormonal Therapies: Using estrogen creams or vaginal tablets for postmenopausal atrophic vaginitis.
Preventive Measures
Preventing vaginal infections requires healthy habits and proactive care. Experts in Thane recommend:
Balanced Diet: Including nutrients, probiotics, and water to support overall health.
Regular Check-Ups: Routine gynecological visits for early detection and management.
Proper Hygiene Practices: Washing with mild, unscented soap and avoiding over-washing or douching.
Why Choose Thane for Vaginal Infection Treatment?
Thane stands out for quality medical care, with professionals like Dr. Aditi Godbole offering holistic solutions. Benefits include:
Personalized Care: Tailored treatment plans addressing individual concerns.
Advanced Diagnostic Techniques: Modern facilities for precise diagnoses.
Expertise and Experience: Skilled specialists with extensive knowledge in gynecological conditions.
For women in Thane, seeking timely medical attention and expert guidance ensures effective management of vaginal infections.
How to Reach Dr. Aditi Godbole’s Clinic in Thane?
Dr. Aditi Godbole’s clinic is conveniently located to serve patients from across Mumbai and beyond.
Clinic Address: Ground Floor, Gaala No. 15, Sai Tirth Towers, Station Rd, Sidharth Nagar, Kopri, Thane East, Thane, Maharashtra 400603
Directions to the Clinic:
Western Line: Take a train to Thane Station. From there, the clinic is just a short 10-minute walk or a 5-minute auto-rickshaw ride.
Central Line: Reach Thane Station via the Central Line, and follow the same directions as above.
Out-of-Mumbai Patients:
By Train: Arrive at Thane Station, well-connected by long-distance trains.
By Road: Use the Eastern Express Highway for a hassle-free journey to Thane East.
By Air: From Mumbai Airport, take a cab or local transport to Thane East, approximately 60-90 minutes away.
The clinic’s accessible location and proximity to Thane Station ensure convenience for all patients.
0 notes
Text
Fluconazole for Dogs: Understanding Its Role in Fungal Treatment
Fungal infections can pose serious health risks to dogs, causing discomfort and complications if not treated promptly. Fluconazole has emerged as a crucial antifungal medication in veterinary medicine, effectively addressing a variety of fungal infections. This article delves into the mechanisms of Fluconazole, the types of infections it treats, how it is administered, potential side effects, and important considerations for dog owners.
What is Fluconazole?
Fluconazole belongs to the triazole class of antifungal medications. It functions by inhibiting the synthesis of ergosterol, a vital component of fungal cell membranes. By disrupting this process, Fluconazole weakens and ultimately kills the fungal cells, helping the immune system eliminate the infection. Its low toxicity and broad spectrum of activity make Fluconazole a preferred choice for treating fungal infections in dogs.
Common Fungal Infections Treated with Fluconazole
Fluconazole is effective against several types of fungal infections, including:
Dermatophyte Infections: These include conditions like ringworm, which primarily affect the skin, causing symptoms such as itching, redness, and hair loss. Fluconazole is often prescribed when topical treatments fail.
Yeast Infections: Malassezia, a type of yeast, can overgrow in certain areas, leading to infections characterized by itching, odor, and inflammation. Fluconazole can provide relief in cases where other treatments are ineffective.
Systemic Fungal Infections: Serious conditions like blastomycosis and coccidioidomycosis can affect multiple organs and require more aggressive treatment. Fluconazole is often a vital part of the treatment regimen for these systemic infections.
When is Fluconazole Prescribed?
Veterinarians may recommend Fluconazole in various circumstances, including:
Failure of Topical Treatments: If a dog’s fungal infection does not respond to topical antifungals, Fluconazole can provide necessary systemic treatment.
Chronic or Recurring Infections: Dogs experiencing persistent fungal or yeast infections may benefit from the consistent approach provided by Fluconazole.
Severe Infections: For serious systemic infections, Fluconazole is frequently included in the treatment plan to help manage and eradicate the infection.
Dosage and Administration
Fluconazole is typically administered orally, available in tablet or liquid form. The veterinarian will determine the appropriate dosage based on the dog’s weight, the type of infection, and its severity. It is essential to follow the veterinarian's instructions closely to ensure effective treatment.
Potential Side Effects
While Fluconazole is generally well-tolerated, pet owners should be aware of possible side effects, including:
Gastrointestinal Upset: Some dogs may experience vomiting, diarrhea, or loss of appetite. If these symptoms persist, contact your veterinarian.
Liver Function Monitoring: Fluconazole can affect liver enzymes. Your veterinarian may recommend regular blood tests to monitor liver function during treatment, especially for long-term use.
Allergic Reactions: Rarely, dogs may exhibit allergic reactions to Fluconazole, showing signs such as swelling, hives, or difficulty breathing. Immediate veterinary assistance is necessary in such cases.
Drug Interactions: Fluconazole may interact with other medications. Always inform your veterinarian about any other treatments your dog is receiving.
Monitoring Treatment Progress
Regular veterinary check-ups are crucial while your dog is on Fluconazole. These appointments allow your veterinarian to monitor the dog’s response to the medication, evaluate any side effects, and make necessary adjustments to the treatment plan.
Important Considerations for Pet Owners
Before starting Fluconazole, consider the following:
Accurate Diagnosis: Ensure your dog receives a thorough diagnosis from a veterinarian. Avoid self-diagnosing or using over-the-counter treatments.
Regular Follow-Ups: Schedule follow-up appointments to monitor your dog’s progress and adapt the treatment plan as needed.
Maintain Hygiene: Keeping your dog’s environment clean can help prevent future fungal infections. Regular grooming and cleaning of bedding are essential practices.
Educate Yourself: Familiarize yourself with the signs of fungal infections so you can seek prompt veterinary care. Early intervention can lead to more successful treatment outcomes.
Conclusion
Fluconazole is an effective treatment for a range of fungal infections in dogs, providing relief and promoting recovery. By understanding how Fluconazole works, the types of infections it addresses, potential side effects, and the importance of monitoring, pet owners can make informed decisions about their dog’s health. If you suspect your dog has a fungal infection or have questions about treatment options, consult your veterinarian. With proper care and treatment, you can help your dog overcome fungal challenges and lead a healthier, happier life.
https://puppadogs.com/fluconazole-for-dogs
0 notes
Text
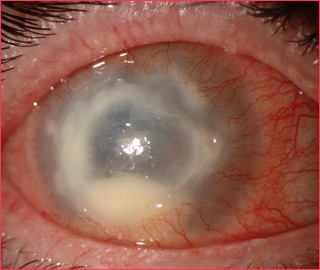

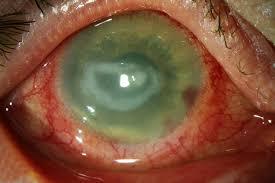
Acanthamoeba Keratitis ... very rare and lead to blindness.
Combination regimens used include:
TMP-SMX, flucytosine, and sulfadiazine
Penicillin G and chloramphenicol (chloramphenicol is no longer available in the United States)
Sulfadiazine, pyrimethamine, and fluconazole
Pentamidine, levofloxacin, amphotericin B, flucytosine, rifampin, and itraconazole
Pentamidine, flucytosine, itraconazole, topical chlorhexidine, and ketoconazole
Pentamidine and itraconazole
Fluconazole, sulfadiazine, and surgical debulking
Ketoconazole, rifampin, and TMP-SMX
TMP-SMX, rifampin, and surgical debulking
Oral and topical miltefosine with intrathecal and systemic amikacin
#family_medicine_review#makkah#mecca#saudi_arabia#family doctors#family physician#general practitioner
0 notes
Text
Understanding Acute Infection: A Comprehensive Overview 🌟
Discover the essential aspects of Acute Infection, including causes, symptoms, diagnosis, and treatment strategies. Learn how to manage and prevent acute infections effectively.
Introduction: What is Acute Infection? 🤔
An Acute Infection is a type of infection that occurs suddenly and is typically characterized by severe symptoms that develop rapidly. Unlike chronic infections, which develop slowly and persist over time, acute infections appear quickly and often require prompt medical attention. These infections can affect various parts of the body, including the respiratory system, gastrointestinal tract, and more.
Understanding the nature of acute infections, their causes, and effective management strategies is crucial for preventing complications and ensuring timely recovery.
Causes of Acute Infection 🌍
Bacterial Infections 🦠
Streptococcus and Staphylococcus: These bacteria can cause acute infections like strep throat and skin infections.
Escherichia coli (E. coli): Often responsible for urinary tract infections and gastrointestinal infections.
Viral Infections 🦠
Influenza Virus: Causes seasonal flu, leading to symptoms such as fever, chills, and muscle aches.
Rhinovirus: Known for causing the common cold, which is typically short-lived but can be intense.
Fungal and Parasitic Infections 🦠
Candida Species: Can cause acute fungal infections like oral thrush and vaginal yeast infections.
Plasmodium Parasites: Responsible for malaria, which presents with acute symptoms including fever and chills.
Symptoms of Acute Infection 🔍
Common Symptoms 🩺
Fever: A sudden increase in body temperature is a common sign of acute infection.
Chills and Sweats: Patients may experience episodes of chills followed by sweating.
Pain and Discomfort: This can include localized pain depending on the area affected, such as a sore throat or abdominal pain.
Severe Symptoms ⚠️
Difficulty Breathing: Indicative of a severe respiratory infection like pneumonia.
Confusion or Altered Mental State: Can occur in severe cases and requires immediate medical attention.
Rapid Heartbeat and Low Blood Pressure: Signs of a potentially serious systemic infection.
Diagnosing Acute Infection 🩺
Medical Evaluation 🔬
Patient History: Detailed history of symptoms, recent travel, and potential exposure to infectious agents.
Physical Examination: A thorough examination to assess symptoms and identify potential sources of infection.
Diagnostic Tests 🧪
Blood Tests: To identify the presence of infection and determine its severity.
Imaging Studies: Such as X-rays or CT scans, to visualize internal infections, especially in cases of suspected pneumonia or abscesses.
Treatment Strategies for Acute Infection 💡
Antimicrobial Medications 💊
Antibiotics: Effective against bacterial infections, prescribed based on the type of bacteria identified.
Antivirals: Used to treat viral infections, such as oseltamivir for influenza.
Antifungals: For fungal infections, medications like fluconazole may be prescribed.
Supportive Care 🌿
Hydration and Rest: Essential for recovery, especially in cases of high fever or gastrointestinal infections.
Pain Management: Medications such as acetaminophen or ibuprofen can alleviate discomfort and fever.
Preventive Measures 🛡️
Vaccination: Regular vaccinations, such as those for influenza, can prevent certain acute infections.
Hygiene Practices: Proper handwashing and avoiding contact with infected individuals can reduce the risk of infection.
Frequently Asked Questions (FAQs) ❓
What is an Acute Infection?
An Acute Infection is an infection that occurs suddenly with severe symptoms and requires prompt medical attention. It contrasts with chronic infections, which develop more slowly and persist over a longer period.
What are the common causes of Acute Infection?
Common causes include bacterial pathogens (like Streptococcus and E. coli), viral agents (such as the influenza virus and rhinovirus), and less frequently, fungal and parasitic organisms.
How is Acute Infection diagnosed?
Diagnosis involves a comprehensive medical evaluation including patient history, physical examination, and diagnostic tests such as blood tests and imaging studies.
What treatment options are available for Acute Infection?
Treatment depends on the cause of the infection and may include antimicrobial medications, supportive care, and preventive measures to avoid recurrence.
How can Acute Infection be prevented?
Preventive measures include vaccinations, practicing good hygiene, and avoiding contact with known sources of infection.
Conclusion: Managing Acute Infections Effectively 🌟
Acute infections require swift and effective management to prevent complications and ensure recovery. By understanding the causes, recognizing symptoms early, and following appropriate treatment and preventive measures, individuals can effectively manage and reduce the impact of these infections.
For further information and resources on managing acute infections, staying informed and consulting healthcare professionals is essential. Your proactive approach to health can make a significant difference in managing and preventing acute infections.
0 notes
Text
The Tinea Pedis Treatment Market is projected to grow from USD 1,490.97 million in 2024 to USD 2,204.52 million by 2032, reflecting a compound annual growth rate (CAGR) of 5.01%.Tinea pedis, commonly known as athlete's foot, is a contagious fungal infection affecting the skin of the feet. It thrives in warm, moist environments, making it prevalent among athletes and individuals who wear closed shoes for extended periods. As awareness of the condition grows, so does the demand for effective treatments, driving significant expansion in the Tinea Pedis treatment market.
Browse the full report at https://www.credenceresearch.com/report/tinea-pedis-treatment-market
Market Overview
The global Tinea Pedis treatment market has witnessed steady growth over the past decade, driven by factors such as increasing awareness of fungal infections, a rise in sports activities, and the availability of over-the-counter (OTC) medications. The market is further bolstered by the growing number of people seeking medical treatment for persistent or recurrent cases of athlete's foot.
According to recent market research, the Tinea Pedis treatment market is expected to continue its upward trajectory, with a compound annual growth rate (CAGR) of around 6% over the next five years. The market is segmented based on treatment type, distribution channel, and region.
Treatment Types
1. Topical Antifungal Agents: Topical treatments dominate the Tinea Pedis treatment market, accounting for a significant share of the market. These include creams, ointments, sprays, and powders that contain antifungal agents like clotrimazole, miconazole, and terbinafine. Topical agents are often the first line of defense against mild to moderate cases of Tinea Pedis due to their ease of use and availability as OTC products.
2. Oral Antifungal Medications: For more severe or resistant cases, oral antifungal medications such as terbinafine, itraconazole, and fluconazole are prescribed. These treatments are usually more effective in eradicating the infection but are associated with a higher risk of side effects, leading to their use primarily under medical supervision.
3. Alternative Treatments: In addition to conventional antifungal therapies, there is growing interest in alternative treatments, including natural remedies like tea tree oil and garlic extract. Although these options are less common, they appeal to consumers looking for natural or complementary therapies.
Distribution Channels
1. Retail Pharmacies: Retail pharmacies represent the largest distribution channel for Tinea Pedis treatments, providing consumers with easy access to OTC medications. The presence of both branded and generic products in pharmacies contributes to the segment's dominance.
2. Online Pharmacies: The online pharmacy segment is experiencing rapid growth, driven by the convenience of home delivery and the increasing trend of online shopping. The availability of detailed product information and customer reviews also supports the growth of this segment.
3. Hospital Pharmacies: Hospital pharmacies are crucial for dispensing prescription medications, particularly for severe cases of Tinea Pedis that require oral antifungal treatments. This segment is expected to maintain steady growth as more patients seek professional medical advice for their condition.
Market Challenges and Opportunities
Despite the growth prospects, the Tinea Pedis treatment market faces challenges such as the risk of side effects from oral medications, the potential for antifungal resistance, and the stigma associated with fungal infections. However, these challenges also present opportunities for innovation.
Pharmaceutical companies are investing in research and development to create more effective and safer treatments, including combination therapies and novel drug delivery systems. Additionally, the rise of telemedicine and e-pharmacies provides new avenues for market expansion, especially in regions with limited access to traditional healthcare facilities.
Key Player Analysis
Bayer AG
Bausch Health Companies Inc. (Valeant Pharmaceuticals, Inc.)
Blueberry Therapeutics Ltd.
Camber Pharmaceuticals, Inc.
CorePharma, LLC
Exeltis USA, Inc.
Glaxosmithkline Plc (GSK)
Glenmark Pharmaceuticals Inc., USA
McKesson (NorthStar Rx LLC)
Novartis AG
Perrigo Company plc
Sebela Pharmaceuticals, Inc.
Taro Pharmaceutical Industries Ltd.
Teva Pharmaceutical Industries Ltd.
Viatris (Mylan N.V.)
Aurobindo Pharma
Segments:
Based on Disease Indication:
Interdigital Tinea Pedis
Plantar Tinea Pedis
Vesicular Tinea Pedis
Based on Route of Administration:
Topical
Gel
Cream
Spray
Lotion
Powder
Oral
Based on Distribution Channel:
Hospital Pharmacies
Retail Pharmacies
Drug Stores
Online Pharmacies
Based on Drug Class:
Antifungals
Combinations
Based on the Geography:
North America
US
Canada
Mexico
Europe
Germany
Uk
France
Italy
Spain
Russia
Rest of Europe
Asia Pacific
China
Japan
India
South Korea
Australia
Rest of Asia Pacific
South America
Brazil
Argentina
Rest of South America
Middle East & Africa
UAE
Saudi Arabia
Qatar
South Africa
Rest of the Middle East & Africa
Browse the full report at https://www.credenceresearch.com/report/tinea-pedis-treatment-market
About Us:
Credence Research is committed to employee well-being and productivity. Following the COVID-19 pandemic, we have implemented a permanent work-from-home policy for all employees.
Contact:
Credence Research
Please contact us at +91 6232 49 3207
Email: [email protected]
Website: www.credenceresearch.com
0 notes
Text
Everything You Need to Know About Thrush Oral Tablets
Thrush oral tablets are medications used to treat oral thrush, a common fungal infection caused by the overgrowth of Candida yeast in the mouth and throat. These tablets contain antifungal agents, such as fluconazole or itraconazole, which work by inhibiting the growth of the Candida fungus. By interfering with the fungal cell membrane or cell wall, thrush oral tablets help to alleviate symptoms such as white patches, soreness, and difficulty swallowing.
Key Ingredients in Thrush Oral Tablets
Thrush oral tablets contain specific antifungal agents that are pivotal in treating oral thrush. Fluconazole is one of the most commonly used ingredients, functioning by disrupting the synthesis of ergosterol, a key component of the fungal cell membrane. Another ingredient, itraconazole, inhibits fungal cell wall synthesis and is effective against a range of fungal infections. Understanding these key ingredients is crucial as they determine the efficacy and safety of the thrush oral tablets.
How to Use Thrush Oral Tablets Effectively?
To use thrush oral tablets effectively, it’s essential to follow the dosage instructions provided by your healthcare provider. Typically, these tablets are taken orally, either with or without food. Adhering to the prescribed dosage and completing the full course of treatment is critical, even if symptoms improve before the medication is finished. Incorrect usage, such as skipping doses or stopping treatment early, can lead to incomplete eradication of the infection and may contribute to the development of drug-resistant strains of Candida. Proper use ensures that the thrush oral tablets fully address the infection and reduce the risk of recurrence.
Potential Side Effects of Thrush Oral Tablets
Common side effects include gastrointestinal issues such as nausea, vomiting, or diarrhea. Some individuals may also experience headaches, dizziness, or rash. Although these side effects are usually mild and temporary, it’s important to monitor them closely. Severe or persistent side effects should be reported to a healthcare provider immediately. Understanding the potential side effects of thrush oral tablets helps in managing them effectively and ensures that you are prepared for any adverse reactions that may occur during treatment.
Comparing Thrush Oral Tablets with Topical Treatments
When treating oral thrush, comparing thrush oral tablets with topical treatments can provide insight into the most suitable approach for your condition. Oral tablets offer systemic treatment, making them ideal for severe or widespread infections. Topical treatments, such as antifungal lozenges or mouthwashes, target the infection directly in the mouth and throat. While they may be effective for mild cases, they might not be as comprehensive as oral tablets.
The Role of Thrush Oral Tablets in Preventing Recurrence
Thrush oral tablets can play a significant role in preventing the recurrence of oral thrush, particularly for individuals who experience frequent outbreaks. For some patients, a healthcare provider may recommend a maintenance dose of thrush oral tablets to prevent future infections. Additionally, addressing and managing underlying conditions that predispose individuals to oral thrush, such as diabetes or immunosuppression, can further help in preventing recurrence. The preventive use of thrush oral tablets, combined with lifestyle and dietary adjustments, can be effective in reducing the likelihood of recurring infections.
Interactions Between Thrush Oral Tablets and Other Medications
Interactions between thrush oral tablets and other medications can impact treatment efficacy and safety. Certain medications, such as anticoagulants or medications used for heart conditions, may interact with antifungal agents, leading to increased risk of side effects or altered drug effectiveness. It’s important to inform your healthcare provider about all other medications and supplements you are taking. This helps in avoiding potential interactions and ensures that the thrush oral tablets are used safely and effectively in conjunction with other treatments.
Cost and Accessibility of Thrush Oral Tablets
The cost and accessibility of thrush oral tablets can vary based on factors such as the specific medication, dosage, and pharmacy. Some antifungal tablets may be available as generic options, which can be more affordable. Insurance coverage and patient assistance programs may also influence the out-of-pocket costs for these medications. Exploring different options and consulting with a pharmacist or healthcare provider can help manage expenses and ensure that you have access to the necessary treatment for oral thrush.
Thrush Oral Tablets for Special Populations
The use of thrush oral tablets in special populations, such as pregnant women or children, requires careful consideration. Certain antifungal medications may not be recommended during pregnancy due to potential risks to the fetus. For children, dosages must be adjusted according to their age and weight. Consulting with a healthcare provider is essential to determine the safest and most effective treatment approach for these populations, ensuring that any potential risks are minimized and the treatment is appropriate for their specific needs.
Future Trends in Thrush Oral Tablet Treatments
Future trends in thrush oral tablet treatments may involve advancements in drug formulations and delivery methods. Research is ongoing to develop new antifungal agents with improved efficacy and fewer side effects. Innovations may include targeted therapies that specifically address Candida infections without affecting beneficial microorganisms. Staying informed about these developments can help in choosing the most current and effective treatment options for managing oral thrush.
Conclusion
Everything You Need to Know About Thrush Oral Tablets provides a comprehensive overview of how these medications work, their key ingredients, and effective usage. By comparing oral tablets with topical treatments, understanding potential side effects, and evaluating their role in preventing recurrence, you can make informed decisions about managing oral thrush.
0 notes
Text
Stuff from OB:
At 38 weeks, induce moms who have GDM so baby doesn't get too big.
Edinburgh Postnatal Depression Scale (EPDS) = depression scale for postpartum pts.
Giving Tdap vaccine at 28 weeks is optimal to give the baby time to absorb the antibodies and not have it wane too much prior to birth.
Between 18-22 weeks, you should be able to feel the baby kick. It takes longer for the mom to feel it if the placenta is more anterior because the placenta can act as a cushion, preventing mom from feeling the kicks.
Hypertensive Moms Love Nifedipine = Hydralazine, Methyldopa, Labetalol, Nifedipine can be used for gestational hypertension. Labetalol and nifedipine are the best.
At 20 weeks the fundal height is at the level of the umbilicus, and then it grows 1 cm per week. If it's greater than or less than 2 cm of expected height, get ultrasound.
Vitamin B6 can help with migraines. Riboflavin and magnesium help with migraines in pregnancy. At 20 weeks, you may start feeling the baby kick. The goal is 20 kicks per hour. If less than 20 kicks/hour, you can not eat or drink something cold, lie down to try to get the baby to move.
Doxylamine (Unisom) and pyridoxine (vitamin B6) can help with nausea after taking every day. Phenergan (Reglan) is first-line for hyperemesis gravidarum. There is a theoretical risk of fetal death in utero with use of Zofran, which has been seen in animals, but not in humans. Zofran a second-line for hyperemesis gravidarum.
Zoloft and Lexapro seem to be best for depression in pregnant women.
If a pt has Nexplanon in and is bleeding for an extended period, you can try an OCP or depot contraceptive for 2 months rather than just taking out Nexplanon.
GDM A1 = diet controlled gestational DM
GDM A2 = insulin controlled gestational DM
Gestational diabetes increases the risk of preeclampsia. Gestational hypertension develops at 20 weeks GA and increases the risk for preeclampsia. An increased BMI and lupus can increase the risk for preeclampsia. Previous history of preeclampsia also increases the risk of preeclampsia. There was a patient who had gestational diabetes which increases her risk of preeclampsia, so is not baseline labs including CMP, urine protein to Cr ratio, started her on aspirin.
Hepatitis C cannot be treated during pregnancy. You can treat the patient postpartum and you test the baby at 3 months. If the viral load is heavy, pt has symptoms, send to peds hepatologist.
The 1st trimester ultrasound is accurate to +/-1 week and in the 2nd week it is accurate 2+/- 2 weeks.
It is safe to treat a yeast infection in a pregnant woman with fluconazole 100 mg once.
You want to obtain the GBS swab at 34-36 weeks. It expires 5 weeks after it is done. Penicillin should be given 2 hours before delivery in patients who are GBS positive.
1st trimester screening includes sexually transmitted infections, Pap only if they need a Pap, CBC, type and screen, Rh factor. Any time you have vaginal bleeding or abortion in a pregnant woman you should give RhoGAM. RhoGAM at 28 weeks and after delivery. Rubella and varicella titers, ultrasound.
if the patient has an increased BMI or glucosuria usually get an early oral glucose tolerance test.
Pregnant women can eat deli meat if they cook it up to 165°, which will kill listeria.
Spotting is normal during the 1st 7-9 weeks of pregnancy.
GDM blood glucose goals: fasting should be less than 95 mg/dL; post-prandial should be 90-140 mg/dL. You should do a 2-hour oral glucose tolerance test 6 weeks after delivery for moms who had GDM (you can also just check a HgbA1c).
Things to know for tests: identifying preeclampsia, gestational vs chronic HTN, risk factors for GDM, management of postpartum hemorrhage, management of hypoglycemia in newborns, management of transient tachypnea of the newborn
4 notes
·
View notes
Text

El fluconazol se usa para tratar infecciones graves por hongos o levaduras, incluida la candidiasis vaginal, candidiasis orofaríngea (aftas, aftas orales), candidiasis esofágica (esofagitis por cándida), otras infecciones por cándida (incluidas infecciones del tracto urinario, peritonitis [inflamación del revestimiento del estómago] e infecciones que pueden ocurrir en diferentes partes del cuerpo) o meningitis por hongos (criptocócica). También se utiliza en niños que reciben un soporte vital llamado oxigenación por membrana extracorpórea (ECMO). Este medicamento actúa matando el hongo o la levadura, o impidiendo su crecimiento.
Consulte a un médico antes de obtener un medicamento.
0 notes
Text
Optimal Dermatologist Strategies for Treating Tinea Infections
Tinea infections, commonly known as ringworm, are fungal infections that can affect the skin, nails, and scalp. Dermatologists employ various effective strategies to diagnose and treat these conditions, tailored to the specific type and severity of the infection. Here, we delve into the most effective dermatologist-recommended strategies for treating tinea infections.
Understanding Tinea Infections
Before exploring treatment strategies, it's crucial to understand tinea infections and their manifestations. Tinea infections, caused by fungi like Trichophyton, Microsporum, and Epidermophyton species, typically appear as circular, red, scaly patches on the skin (ringworm), but can also affect the nails (onychomycosis) and scalp (tinea capitis).
Diagnosis by Dermatologists
Accurate diagnosis is critical for effective treatment. Dermatologists usually diagnose tinea infections through clinical examination, reviewing medical history, and sometimes using laboratory tests such as skin scrapings or fungal cultures. This helps determine the specific fungus causing the infection and its severity.
Optimal Treatment Approaches for Tinea Infections
Topical Antifungal Medications: For mild to moderate cases, dermatologists often recommend topical antifungal creams, lotions, or powders. These medications, such as clotrimazole, terbinafine, or miconazole, are applied directly to the affected area and work by killing the fungus or inhibiting its growth.
Oral Antifungal Medications: In more extensive or resistant cases, dermatologists may prescribe oral antifungal medications. Examples include fluconazole or griseofulvin, which are taken orally and circulate through the bloodstream to reach the affected areas.
Combination Therapies: For severe or persistent infections, dermatologists may suggest a combination of topical and oral antifungal treatments. This comprehensive approach ensures effective treatment and faster symptom relief.
Adjunct Therapies: Alongside antifungal medications, dermatologists may recommend adjunct therapies to manage symptoms and prevent recurrence. This may include using medicated shampoos for tinea capitis, maintaining cleanliness and dryness of affected areas, and avoiding sharing personal items like towels or clothing.
Follow-Up and Monitoring: Dermatologists stress the importance of follow-up appointments to monitor treatment progress and ensure complete resolution of the infection. They also provide guidance on preventive measures to minimize the risk of reinfection or spreading the fungus.
Read more…
0 notes
Text
Dermatology Prescription Medications: A Comprehensive Guide

Dermatology, the branch of medicine dealing with the skin, hair, and nails, encompasses a wide array of conditions and treatments. Prescription medications play a crucial role in managing various dermatological issues, ranging from acne and eczema to psoriasis and skin infections. This article delves into the diverse world of dermatology prescription medications, highlighting their uses, benefits, and potential side effects.
Understanding Dermatology Prescription Medications
Dermatology prescription medications are drugs prescribed by a dermatologist to treat skin-related conditions. These medications can be topical (applied directly to the skin) or systemic (taken orally or injected). The choice of medication depends on the specific condition, its severity, and the patient's overall health.
Common Dermatological Conditions and Their Treatments
Acne Vulgaris
Topical Retinoids: Medications such as tretinoin and adapalene are derivatives of vitamin A. They work by promoting cell turnover and preventing the clogging of hair follicles.
Antibiotics: Topical antibiotics like clindamycin and erythromycin help reduce bacteria and inflammation on the skin. Oral antibiotics, such as doxycycline and minocycline, may be prescribed for more severe cases.
Benzoyl Peroxide: Often combined with antibiotics, benzoyl peroxide has antibacterial properties and helps to prevent resistance to antibiotics.
Hormonal Treatments: For females, oral contraceptives and anti-androgens like spironolactone can be effective in managing acne related to hormonal imbalances.
Eczema (Atopic Dermatitis)
Topical Corticosteroids: Hydrocortisone, betamethasone, and clobetasol are commonly used to reduce inflammation and itching. The potency of the corticosteroid depends on the severity of the eczema.
Calcineurin Inhibitors: Tacrolimus and pimecrolimus are non-steroidal medications that modulate the immune response and reduce inflammation.
Systemic Immunosuppressants: For severe cases, drugs like cyclosporine and methotrexate may be prescribed to suppress the immune system and control symptoms.
Psoriasis
Topical Treatments: Calcipotriene, a vitamin D analog, and topical corticosteroids are frequently used to manage mild to moderate psoriasis.
Biologic Agents: These are advanced treatments targeting specific parts of the immune system. Examples include adalimumab, etanercept, and ustekinumab.
Systemic Treatments: Methotrexate, cyclosporine, and acitretin are oral medications used for more severe cases.
Rosacea
Topical Treatments: Metronidazole and azelaic acid help reduce redness and inflammation.
Oral Antibiotics: Doxycycline and minocycline are commonly used to manage moderate to severe rosacea.
Other Treatments: Ivermectin cream and brimonidine gel can help with specific symptoms like inflammatory lesions and redness, respectively.
Fungal Infections
Topical Antifungals: Clotrimazole, miconazole, and terbinafine are used to treat fungal infections of the skin.
Oral Antifungals: For more extensive infections, oral medications like fluconazole, itraconazole, and terbinafine may be necessary.
Mechanisms of Action
The effectiveness of dermatology prescription medications lies in their diverse mechanisms of action:
Anti-inflammatory Agents: Many skin conditions are inflammatory in nature. Corticosteroids and non-steroidal medications like calcineurin inhibitors reduce inflammation and alleviate symptoms.
Antibacterial and Antifungal Agents: These medications, such as antibiotics and antifungals, target and eliminate pathogenic bacteria and fungi causing infections.
Immunomodulators: Biologics and systemic immunosuppressants modify the immune response, which is particularly beneficial in autoimmune conditions like psoriasis and severe eczema.
Cell Turnover Regulators: Retinoids and similar agents increase cell turnover, preventing clogged pores and reducing lesions in acne and psoriasis.
Side Effects and Considerations
While dermatology prescription medications can be highly effective, they are not without potential side effects. Understanding these is crucial for safe and effective treatment.
Topical Medications
Skin Irritation: Many topical medications can cause redness, burning, or peeling, especially during the initial stages of treatment.
Allergic Reactions: Some patients may develop allergic reactions to topical medications, characterized by increased redness, itching, and swelling.
Systemic Medications
Antibiotics: Long-term use can lead to antibiotic resistance and disrupt the normal flora, potentially causing secondary infections.
Immunosuppressants: These can increase the risk of infections and may have systemic side effects like liver toxicity and hypertension.
Biologics: While generally well-tolerated, biologics can sometimes cause injection site reactions and increase the risk of infections due to immune suppression.
Retinoids
Teratogenicity: Oral retinoids are highly teratogenic and can cause severe birth defects. Women of childbearing age must use effective contraception.
Dryness and Sensitivity: Both topical and oral retinoids can cause significant dryness and sensitivity to sunlight.
Advances in Dermatology Medications
Recent advancements have significantly expanded the arsenal of dermatology medications. Biologics and new small-molecule drugs offer targeted therapy with fewer side effects compared to traditional treatments. Additionally, research into the skin microbiome is opening up new avenues for treating various skin conditions by modulating the skin's natural bacterial environment.
Conclusion
Dermatology prescription medications are essential tools in managing a wide range of skin conditions. They work through various mechanisms to address the underlying causes and symptoms of dermatological diseases. However, their use requires careful consideration of potential side effects and individual patient factors. With ongoing advancements in dermatology, the future holds promise for even more effective and personalized treatments, improving the quality of life for patients worldwide.
In summary, understanding the options, mechanisms, and considerations associated with dermatology prescription medications can empower patients and healthcare providers to make informed decisions and achieve the best possible outcomes in skin health.
0 notes
Text
Understanding Nail Fungus: Treatment Methods and Recommendations
Introduction:
Onychomycosis, a widespread ailment that affects millions of individuals worldwide, is the medical term for nail fungus. It shows up as thickness, discoloration, and detachment of the nail from the nail bed. The fungus that cause this infection prefer warm, humid conditions, which makes toenails especially vulnerable. Not only is effective therapy important for appearance, but it also helps stop more problems from arising. The two main forms of treatment that are examined in this article are Oral antifungal medication and nail lotions.

Topical Solutions: Nail Fungal Creams
When treating mild to moderate nail fungal infections, topical antifungal medications are frequently utilized. The afflicted nails and surrounding skin are treated immediately with these lotions or ointments. The following are a few of the most often prescribed topical antifungal drugs:
Ciclopirox:
Sold as a nail lacquer, ciclopirox is applied once daily to affected nails. The treatment can last up to 48 weeks and works by suppressing the growth of fungus. Finaconazole:
Applied once a day for 48 weeks, this relatively new topical medication. It is renowned for having a higher penetration rate into the nail bed than certain other treatments.
Tavaborole:
Another topical antifungal that must be used daily for up to a year, tavaborole is administered similarly to ciclopirox and efinaconazole.
Topical therapies typically cause little adverse effects, such as redness and localized discomfort, and are well tolerated. However, because it might be challenging to penetrate the tough nail surface and get to the underlying fungus, its efficacy may be restricted.
Oral Antifungal Drugs: Systematic Method
Oral antifungal medicines are frequently used for severe or persistent infections. Because the active chemicals are delivered to the illness site through the bloodstream, these systemic therapies have a higher success rate. Antifungal drugs that are often taken orally include:
Terbinafine:
Typically used once daily for six to twelve weeks, terbinafine builds up in the nail bed and continues to work long beyond the course of treatment. With a 70% cure rate, it is incredibly effective.
Itraconazole:
This drug can be used continuously for three months or in pulse doses of one week every month. It functions by interfering with the fungal cell membrane's production. Fluconazole:
Although less frequently recommended, fluconazole is a viable therapeutic option for nail fungus, particularly for individuals who are not responding to conventional therapies. Typically, it is taken once a week for a few months. The adverse effects of oral antifungal drugs can include headaches, stomach problems, and, in rare instances, liver damage. As a result, in order to watch for any negative effects, patients receiving oral antifungal medication frequently need to have periodic liver function tests.
Adjunct Treatments Using Combination Therapy
Combining topical and oral medicines can sometimes increase the likelihood of completely curing the infection. Patients with persistent or severe infections may benefit most from this technique. Furthermore, non-pharmacological interventions like laser therapy are becoming more and more popular as adjuvant measures. Using concentrated light, laser treatment eliminates the fungus without causing harm to the surrounding tissue. Even if it seems promising, more studies are required to determine its effectiveness and long-term results.
Keeping Nail Fungus at Bay
Prevention is an important element of controlling nail fungus, especially for people who are prone to recurring infections. Important preventive actions include of:
Keeping dry and clean feet
Donning moisture-wicking socks and ventilated shoes
Steer clear of bare feet in public spaces like locker rooms and swimming pools.
Regularly washing and cutting nails
Applying antifungal sprays or powders to shoes
Recognizing the Signs of Fungal Nails
Recognizing nail fungus symptoms early on can considerably improve treatment results. Common indications of onychomycosis consist of:
Nail discoloration (white, yellow, or brown)
Thickness of the nail Chipped or uneven surface
distorted form of the nails
nail breaking off from the nail bed
Bad smell
To stop the infection from spreading and causing more serious damage, prompt identification and treatment are essential.
Risk Factors for the Development of Nail Fungi
There are a number of risk factors that raise the possibility of nail fungus. Recognizing these can aid in early detection and prevention: Age: Due to slower nail development and decreased blood circulation, older persons are more susceptible to nail fungus. Medical Conditions: Sickness such as psoriasis, diabetes, and compromised immune systems might make a person more vulnerable. Lifestyle: People who often use public swimming pools or showers, such as athletes, are more likely to be at risk. Shoes: Wearing shoes that are too tight or airtight can foster the growth of fungi. Alternative Medicines and Home Remedies While pharmaceutical drugs are frequently required to treat nail fungus, there are certain natural cures and complementary therapies that help speed up recovery or stop recurrence.
Home Remedy and Alternative Treatments
While pharmaceutical drugs are frequently required to treat nail fungus, there are certain natural cures and complementary therapies that help speed up recovery or stop recurrence: Tea Tree Oil: You can apply tea tree oil to the damaged nail because of its antifungal qualities. Vinegar Soaks: Soaking feet in a vinegar and water solution can help inhibit the formation of fungi. Garlic: There are antifungal benefits to applying crushed garlic or garlic oil to the affected region. Oregano Oil: Thymol, an antifungal and antibacterial compound, is present in this essential oil. Although these treatments have their uses, they are usually not as successful as medical interventions for serious infections.
When to Seek Advice from a Medical Professional
If you think you may have a fungal infection in your nails, you should definitely consult a doctor, especially if:
The illness is getting worse or spreading.
either have diabetes or a compromised immune system.
Over-the-counter medications don't work.
You feel a great deal of pain or discomfort.
A medical professional is qualified to make an accurate diagnosis and suggest the best course of action.
Conclusion:
Nail fungus is a chronic and often frustrating problem, but with the right combination of nail fungal treatments, oral antifungal drugs, or both, it can be properly managed. To ascertain the best course of action based on the severity of their infection and general health, patients should speak with medical professionals. To prevent reinfection and preserve healthy nails, prevention techniques are equally crucial. Early symptom recognition, knowledge of risk factors, and investigation of medical and non-medical remedies can enable people to effectively and pro-actively treat nail fungus.
0 notes
Text
Understanding Acute Infection: A Comprehensive Overview 🌟

Discover the essential aspects of Acute Infection, including causes, symptoms, diagnosis, and treatment strategies. Learn how to manage and prevent acute infections effectively.
Introduction: What is Acute Infection? 🤔
An Acute Infection is a type of infection that occurs suddenly and is typically characterized by severe symptoms that develop rapidly. Unlike chronic infections, which develop slowly and persist over time, acute infections appear quickly and often require prompt medical attention. These infections can affect various parts of the body, including the respiratory system, gastrointestinal tract, and more.
Understanding the nature of acute infections, their causes, and effective management strategies is crucial for preventing complications and ensuring timely recovery.
Causes of Acute Infection 🌍
Bacterial Infections 🦠
Streptococcus and Staphylococcus: These bacteria can cause acute infections like strep throat and skin infections.
Escherichia coli (E. coli): Often responsible for urinary tract infections and gastrointestinal infections.
Viral Infections 🦠
Influenza Virus: Causes seasonal flu, leading to symptoms such as fever, chills, and muscle aches.
Rhinovirus: Known for causing the common cold, which is typically short-lived but can be intense.
Fungal and Parasitic Infections 🦠
Candida Species: Can cause acute fungal infections like oral thrush and vaginal yeast infections.
Plasmodium Parasites: Responsible for malaria, which presents with acute symptoms including fever and chills.
Symptoms of Acute Infection 🔍
Common Symptoms 🩺
Fever: A sudden increase in body temperature is a common sign of acute infection.
Chills and Sweats: Patients may experience episodes of chills followed by sweating.
Pain and Discomfort: This can include localized pain depending on the area affected, such as a sore throat or abdominal pain.
Severe Symptoms ⚠️
Difficulty Breathing: Indicative of a severe respiratory infection like pneumonia.
Confusion or Altered Mental State: Can occur in severe cases and requires immediate medical attention.
Rapid Heartbeat and Low Blood Pressure: Signs of a potentially serious systemic infection.
Diagnosing Acute Infection 🩺
Medical Evaluation 🔬
Patient History: Detailed history of symptoms, recent travel, and potential exposure to infectious agents.
Physical Examination: A thorough examination to assess symptoms and identify potential sources of infection.
Diagnostic Tests 🧪
Blood Tests: To identify the presence of infection and determine its severity.
Imaging Studies: Such as X-rays or CT scans, to visualize internal infections, especially in cases of suspected pneumonia or abscesses.
Treatment Strategies for Acute Infection 💡
Antimicrobial Medications 💊
Antibiotics: Effective against bacterial infections, prescribed based on the type of bacteria identified.
Antivirals: Used to treat viral infections, such as oseltamivir for influenza.
Antifungals: For fungal infections, medications like fluconazole may be prescribed.
Supportive Care 🌿
Hydration and Rest: Essential for recovery, especially in cases of high fever or gastrointestinal infections.
Pain Management: Medications such as acetaminophen or ibuprofen can alleviate discomfort and fever.
Preventive Measures 🛡️
Vaccination: Regular vaccinations, such as those for influenza, can prevent certain acute infections.
Hygiene Practices: Proper handwashing and avoiding contact with infected individuals can reduce the risk of infection.
Frequently Asked Questions (FAQs) ❓
What is an Acute Infection?
An Acute Infection is an infection that occurs suddenly with severe symptoms and requires prompt medical attention. It contrasts with chronic infections, which develop more slowly and persist over a longer period.
What are the common causes of Acute Infection?
Common causes include bacterial pathogens (like Streptococcus and E. coli), viral agents (such as the influenza virus and rhinovirus), and less frequently, fungal and parasitic organisms.
How is Acute Infection diagnosed?
Diagnosis involves a comprehensive medical evaluation including patient history, physical examination, and diagnostic tests such as blood tests and imaging studies.
What treatment options are available for Acute Infection?
Treatment depends on the cause of the infection and may include antimicrobial medications, supportive care, and preventive measures to avoid recurrence.
How can Acute Infection be prevented?
Preventive measures include vaccinations, practicing good hygiene, and avoiding contact with known sources of infection.
Conclusion: Managing Acute Infections Effectively 🌟
Acute infections require swift and effective management to prevent complications and ensure recovery. By understanding the causes, recognizing symptoms early, and following appropriate treatment and preventive measures, individuals can effectively manage and reduce the impact of these infections.
For further information and resources on managing acute infections, staying informed and consulting healthcare professionals is essential. Your proactive approach to health can make a significant difference in managing and preventing acute infections.
1 note
·
View note